CORTICOSTEROIDS AND YOUR CHRONIC PAIN
“Corticosteroids are perhaps the most enigmatic of all the drugs in the western medicine man’s arsenal. It has been said by many practitioners that they are the most used and most abused of all our medicines. Corticosteroids are a necessary component of a healthy physiology and they can be life saving…or they can cause multiple adverse side effects that can be devastating to a dog’s health and well-being. Since this class of biochemicals affects nearly all cells of the body, their beneficial effects can be widespread – and their adverse effects may be totally debilitating and long-lasting.” Dr. Randy Kidd from his article, Use Corticosteroids On Your Canine With Caution
“Long-term corticosteroid use may be associated with more serious sequel, including osteoporosis, aseptic joint necrosis, adrenal insufficiency, gastrointestinal, hepatic, and ophthalmologic effects, hyperlipidemia, growth suppression, and possible congenital malformations.” The conclusions of a study from a 2001 issue of the Journal of Clinical Gastroenterology (Side Effects of Corticosteroid Therapy)
“Medications like dexamethasone, methylprednisolone and prednisone have a long list of serious side effects. They include fluid retention, hypertension, headache, increased susceptibility to infection, muscle weakness, diabetes, osteoporosis, tendon rupture, glaucoma, cataracts and ulcers. Psychological reactions such as anxiety, irritability, mood swings, insomnia, confusion and psychosis are disorienting at best and disabling at worst.
Many physicians have been led to believe that a week or two of a drug like prednisone poses very little risk. That is why they are often quite reassuring to patients who may worry about corticosteroid side effects. A new study reveals that even short-term steroid use can trigger dangerous side effects.” From a May 2017 episode of the People’s Pharmacy
Because THE BIG FIVE is standard medical fare for people struggling with CHRONIC PAIN, you should know what these drugs (along with any others you may be taking) are doing to you. Today we talk about one of the ‘Big Five’s’ heavy-hitters — corticosteroids (aka glucocorticoids). For a very long time I’ve been telling you that when it comes to chronic pain and disease, inflammation is everything (HERE). I’ve also shown you that IMMUNE SYSTEM SUPPRESSION is the number one medical therapy in America.
These facts become far more relevant once you realize two things. Firstly that inflammation is an immune system response, and secondly that a certain degree of inflammation is necessary for you to be able to heal damaged tissues, wherever those tissues may be.
When you understand how corticosteroids work, and then look at the research, you might find it surprising just how commonly these drugs are prescribed. What’s truly amazing is that while many physicians continue to use corticosteroids (Cortisone and similar) in the same way they’ve been using them for the past three decades, a large and growing part of the medical community has been sounding the alarm.
One of the best examples of this came from MY PATHOLOGY TEXTBOOK (written by physicians from the University of Texas and University of North Carolina). These renowned pathologists were raising the Jolly Roger concerning corticosteroids thirty years ago. And they weren’t the only ones — not by a long shot.
I’ve not only shown you how (and why) much of what’s found in the biomedical peer-review cannot be trusted (HERE), I’ve shown you that in similar fashion to numerous other medical arenas (HERE are a few of them), corticosteroids are not being used according to medical guidelines (HERE). While many people — especially short term users — will get away with this, there is frequently a price to be paid. Why? Simply because corticosteroids, while unarguably having potent anti-inflammation qualities, also happen to destroy / deteriorate collagen-based tissue (bone, cartilage, FASCIA, TENDONS, ligaments, muscle, etc, etc).
In other words, using corticosteroids essentially means that you are trading tomorrow for today —- short term relief for long-term degeneration and dysfunction. Although a book could easily be written on the subject, allow me to give you a small taste of what I’m talking about.
There are several important points to grasp before getting into the meat of today’s post. Firstly is that although they are endocrinologically related, do not confuse CORTICOSTEROIDS (potent anti-inflammatories such as cortisone and prednisone) with anabolic steroids — muscle building drugs that can help make strength athletes and bodybuilders huge. Secondly, as you read about the side effects, never forget that hundreds of studies on Adverse Events (AE’s — the medical word for side effects) have shown that on average, they are reported to the proper authorities only about 1% of the time (HERE, HERE, and HERE).
What this does is give most pharmaceutical drugs safety profiles that are not nearly as good in the real world as is touted in the individual studies you’ll see below. Thirdly, be aware that there are NUMEROUS WAYS that Big Pharma is cooking their books in order to make their products look better (the chief one being not publishing research that shows their products in a negative light — see link). And fourthly, it is shocking how many studies — particularly older studies — did not look at side effects as a matter of course. In many cases, if researchers were not specifically studying side effects, they were not dealt with or mentioned in the study’s results.
- CORTICOSTEROIDS AFFECT YOUR WOUND-HEALING CAPABILITIES: An editorial in the journal Wounds (Corticosteroids and Wound Healing) revealed that anything over 10 days is considered “long term” corticosteroid use. The same study concluded that, “It has been found that corticosteroids influence all phases of wound healing“. This means that if you were taking steroids for that WHIPLASH INJURY your were in three months ago, you essentially affected ALL FOUR PHASES of the healing process. The author went on to say that, “The chronic treatment with corticosteroids presents different hazards for wound healing. Chronic corticosteroid use is defined as taking the drug at doses of greater than 10 mg/kg of body weight for more than 1 week. Patients treated for 30 days prior to wounding or an operative procedure were reported to have had a 2-fold increase in wound infection, 2 to 3 times higher incidence of wound dehiscence [a surgical complication in which a wound ruptures along a surgical incision], and a 4 times greater mortality compared to those not taking steroids for that period of time. In another study, rheumatoid arthritis patients taking corticosteroids and having joint replacement surgery had a significantly higher incidence of delayed wound healing if they had taken the steroids for more than 3 years compared to those who had taken the drug for less than 3 years. Obviously, chronic corticosteroid therapy will present a problem with wound healing.“
- SHORT-TERM CORTICOSTEROID USE CAN CAUSE SERIOUS HEALTH ISSUES: For decades, physicians have been telling patients that while it’s true that long-term corticosteroid use is problematic, short term use is no big deal — it’s safe. That is until a study published in March’s issue of the British Medical Journal (Short Term Use of Oral Corticosteroids and Related Harms Among Adults in the United States) looked at over 1.5 million individuals both before and after starting a month or less of oral steroids. The authors concluded that things like fractures, blood clots, and infections, carried an “increased risk of adverse events. Corticosteroids are also used often in the short term to treat many other prevalent conditions where evidence is lacking, such as non-specific musculoskeletal pain and rashes. Incidence rates of sepsis, venous thromboembolism, and fracture were statistically significantly higher in short term users of oral corticosteroid than in non-users. The incidence was approximately 7% for short term oral corticosteroid use…..” What that means, folks, is that about 1 in 11 of you taking short term steroids are going to have something bad happen.
- PEOPLE WILL KNOW YOU ARE ON STEROIDS: One of the most common side effects of corticosteroids is water retention, which occurs all over, but most noticeably in the face. People on corticosteroids frequently end up with what’s known as “moon face” to go along with the weight gain that you will see in another bullet point”.
- CORTICOSTEROIDS AND BONE LOSS / OSTEOPOROSIS: One of the more well known side effects of taking corticosteroids is OSTEOPOROSIS. A study from Clinical Endocrinology, published clear back in 1989 (Pathogenisis and Treatment of Steroid Osteoporosis) concluded that, “Prospective studies of bone mass during steroid treatment confirm that these drugs do cause progressive bone loss. Comparable studies in asthmatic patients have found dose-related losses of peripheral trabecular bone of between 1 and 7% per annum. The first line of prophylaxis against this potentially disabling side-effect of glucocorticoid therapy [osteoporosis] must remain the use of the lowest steroid dose for the shortest possible period.” The April issue of the Journal of Allergy and Clinical Immunology (Oral Corticosteroid Exposure and Adverse Effects in Asthmatic Patients) confirmed this when they stated, “Although previous research has documented the deleterious effect of continuous oral corticosteroid exposure in patients with severe asthma, our results suggest that each oral corticosteroid prescription might result in a cumulative burden on current and future health regardless of dose and duration.” There are hundreds of similar studies, each one scarier than the one before it.
- CORTICOSTEROIDS AND INFECTIONS: I am not going to spend any time on this bullet because there are hundreds of studies on the topic. Suffice it to say that when you suppress the immune system, infections of all kind increase dramatically.
- CORTICOSTEROIDS SERIOUSLY AND ADVERSELY AFFECT THE BRAIN: I was all of 14 years old when the Archives of General Psychiatry published Side Effects of Corticosteroid Therapy Psychiatric Aspects —- back in 1981. Listen to their freaky conclusions. “Euphoria, depression, and psychotic reactions are the common manifestations of corticosteroidinduced mental disturbances; females seem to be more prone to these disturbances than male. At present there are no simple models to explain the psychotic reactions, anxiety, or agitation seen in corticosteroid-induced mental disturbances.” In 2006, the Mayo Clinic published a paper called Psychiatric Adverse Effects of Corticosteroids in which they stated, “Corticosteroids have become the cornerstone of therapy for many neurologic, respiratory, gastrointestinal, renal, endocrine, hematologic, neoplastic, rheumatologic, dermatologic, ophthalmic, and allergic conditions. More than 10 million new corticosteroid prescriptions are filled each year, with up to 0.9% of the general population and as many as 7% of hospitalized patients receiving oral corticosteroid therapy at any given point. The most frequently identified symptoms include agitation, anxiety, distractibility, fear, hypomania, indifference, insomnia, irritability, lethargy, labile mood, pressured speech, restlessness, and tearfulness. The most commonly reported corticosteroid-induced psychiatric disturbances are affective, including mania, depression, or mixed states. Most often, patients receiving short-term corticosteroid therapy present with euphoria or hypomania, whereas long-term therapy tends to engender depressive symptoms. Although mood disorders occur in the vast majority of cases, either delirium or frank psychosis, typified by hallucinations, delusions, and disorganized thought, is the presenting syndrome in a sixth of patients. Severe episodes of depression, mania, or psychosis frequently include suicidal ideation.“
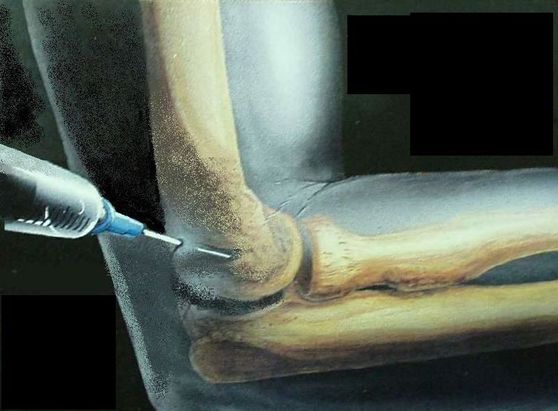
- ELBOW TENDINITIS / TENDINOSIS (EPICONDYLITIS) AND CORTICOSTEROIDS: Back in 2013, one of the publications of the British Medical Journal (BMJ Open) did a systematic review on the subject, concluding that, “Corticosteroid injection gave a short-term reduction in pain versus no intervention or non-steroidal anti-inflammatory drugs. At intermediate follow-up, we found an increase in pain, reduction in grip strength, and negative effect on overall improvement. Corticosteroid injections have a short-term beneficial effect on lateral epicondylitis, but a negative effect in the intermediate term.” Why might this be? It’s why even when cortisone shots relieve your pain, your doctor will tell you you can’t have very many. Earlier this month, the International Journal of Applied and Basic Medical Research published a study (Autologous Platelet-Rich Plasma Versus Corticosteroid in the Management of Elbow Epicondylitis) that essentially confirmed these findings and went a step further, providing information on an alternative. “Epicondylitis is the most common problem of the elbow in the age group between 35 and 54 years. Histologic specimens from chronic cases confirm that tendinitis is not an acute inflammatory condition but rather a failure of the normal tendon repair mechanism associated with angiofibroblastic degeneration. Tendon regeneration may be improved by injecting autologous growth factors obtained from the patient’s own blood. Autologous growth factors can be injected with autologous whole blood or platelet-rich plasma (PRP).” Although I am intrigued by PRP INJECTIONS, I have not really seen it work in many people. For more information on elbow pain, read about how to effectively deal with LATERAL EPICONDYLITIS (Tennis Elbow) or MEDIAL EPICONDYLITIS (Golfer’s Elbow).
- CORTICOSTEROIDS FOR PLANTAR FASCIITIS: For those of you who have struggled with it, you already know that PLANTAR FASCIITIS can be debilitating. For as long as I’ve been in practice, the number one treatment for those going to doctors / podiatrists for PF is whatever else, along with a corticosteroid injection. Not only does this dramatically increase your chance of a very nasty and long-healing injury (ruptured Achilles tendon), but according to the gold-standard of medical reviews it doesn’t work well either. After looking at 39 studies on the topic, the COCHRANE REVIEW (Injected Corticosteroids for Treating Plantar Heel Pain in Adults) concluded that, “We found low quality evidence that local steroid injections compared with placebo or no treatment may slightly reduce heel pain up to one month but not subsequently.”
- CORTICOSTEROIDS AND CARPAL TUNNEL SYNDROME: In a study that recommended corticosteroids for CARPAL TUNNEL SYNDROME (Carpal Tunnel Syndrome: Initial Management and the Treatment of Recalcitrant Patients) from the February issue of Instructional Course Lectures, the authors showed what many before them have shown. The Carpal Tunnel Surgery many times does not work. “Patients with recurrent symptoms often have perineural fibrosis that tethers the median nerve.” Did I see the word “TETHERS“? After invoking Carpal Tunnel Syndrome, last November’s issue of Seminars in Radiology (Injectable Corticosteroids: Take Precautions and Use Caution) stated, “Corticosteroids carry a low risk of complications but commonly cause systemic and local adverse effects.” In other words, you probably won’t die, but these drugs are associated with a ton of side effects, both at the spot of injection and throughout your body.
- GLUCOCORTICODS (CORTICOSTEROIDS) AND RHEUMATOID ARTHRITIS: RA is an autoimmune disease where one’s own immune system attacks its own joint cartilage. In yet another meta analysis by Cochrane (Glucocorticoids for Rheumatoid Arthritis), the authors showed that even though the steroids slowed down the erosive progression of the disease over the first two years, “Harms were not reviewed. There remains concern about potential long-term adverse reactions to glucocorticoid therapy, such as increased cardiovascular risk“. It seems strange to me that the mighty Cochrane did a review without taking into account side effects. However, many other studies I found specifically talked about Rheumatoid because so many people struggling with this disease are on steroids for the duration.
- CORTICOSTERODS FOR HEAD INJURES: AHC Media published an article by ER physician and professor, Stephanie Abbuhl, called Steroid Infusion May Be Harmful in Acute Head Injury. After looking at a study from Lancet that oversaw 10,000 head injury cases that were either given steroids or placebo after serious head injuries, she stated, “The risk of death from all causes within two weeks was higher in the group allocated corticosteroids when compared with the placebo group.” She went on to reveal why this is important. “The authors report that a 1995 survey showed that 64% of trauma centers in the United States used corticosteroids more than half the time in the intensive care management of head injury patients. Although controversial, the standard of care has been to treat acute blunt spinal cord injury with methylprednisolone since the National Acute Spinal Cord Injury Studies showed slight neurologic improvement with this treatment…“
- CORTICOSTEROIDS FOR COMPLICATIONS OF THE FLU: Despite getting their ANNUAL FLU SHOTS (and despite any real evidence these work), some people — particularly the elderly or those who are immunocompromised — end up in the hospital with complications (HERE). A recent Cochrane Review on the subject stated, “These patients are often prescribed steroids as part of their treatment, although the evidence that steroids are beneficial in these circumstances is controversial. We found that patients with influenza who received additional steroid treatment might have had a greater risk of death compared to patients who did not receive steroid treatment. Hospital-acquired infection was the main ‘side effect.” Think about why this would be. Corticosteroids are powerful immune system suppressors.
- CORTICOSTEROID INJECTIONS IN THE SOFT TISSUES: After looking at hundreds of studies going back into the mid fifties, a huge review in a 2010 issue of BMC Musculoskeletal Disorders (Adverse Effects of Extra-Articular Corticosteroid Injections: A Systematic Review) concluded that, “The local effects consisted of local pain, degeneration, atrophy and change in skin colour, local infection, impact on collagen metabolism expressed as tendon ruptures, and perilymphatic atrophy.” The overall rate of these side effects was reported to be about 6%.
- CORTICOSTEROIDS FOR TRIGGER POINTS: Although this has been popular for years, once you understand what TRIGGER POINTS are and how DRY NEEDLING works, you’ll start to realize that corticosteroids are not the best option — especially in light of the previous bullet point.
- CORTICOSTEROIDS FOR BACK PROBLEMS: A two month old study published in the Annals of Internal Medicine (Intradiscal Glucocorticoid Injection for Patients With Chronic Low Back Pain Associated With Active Discopathy) looked at the effects of corticosteroid injections on disc herniations. Despite this being the “go to” therapy, we saw the same theme we’ve seen over and over again. Short term relief without long-term benefit. “In chronic LBP associated with active discopathy, a single glucocorticoid inter-discal injection reduces LBP at 1 month but not at 12 months.” The April issue of the Archives of Physical Medicine and Rehabilitation (Long-Term Effects of Repeated Injections of Local Anesthetic With or Without Corticosteroid for Lumbar Spinal Stenosis) concluded that when it comes to SPINAL STENOSIS, “For lumbar spinal stenosis symptoms, epidural injections of corticosteroid plus lidocaine offered no benefits from 6 weeks to 12 months beyond that of injections of lidocaine alone in terms of self-reported pain and function or reduction in use of opioids and spine surgery. Repeated injections of either type offered no additional long-term benefit if injections in the first 6 weeks did not improve pain.” When it comes to disc problems (DEGENERATIVE DISCS or HERNIATED DISCS) causing CHRONIC LOW BACK PAIN, steroid shots have always been the treatment-of-choice. The April issue of the Annals of Internal Medicine (Intradiscal Glucocorticoid Injection for Patients With Chronic Low Back Pain Associated With Active Discopathy) came to similar conclusions. “In chronic LBP associated with active discopathy, a single glucocorticoid intradiscal injection reduces LBP at 1 month but not at 12 months.” Yet again, short term relief is traded for long-term degeneration. By the way, the previous link shows you what it takes to address these and other back issues on your own.
- CORTICOSTEROIDS AND TRIGGER FINGERS: Trigger fingers are common as hardworking people get older. A study from this month’s issue of the Journal of Hand Surgery: European Volume (Evidence-Based Management of Adult Trigger Digits) concluded that, “when compared with surgery, there is strong evidence that corticosteroid injection is associated with increased rates of ongoing or recurrent symptoms at 6 months after intervention.”
- CORTICOSTEROIDS FOR HIP PROBLEMS: While this has been the standard of care for decades, should it be in light of what we know? The April issue of the Journal of Sports and Physical Therapy (Dry Needling Versus Cortisone Injection in the Treatment of Greater Trochanteric Pain Syndrome) removes any doubt. “Greater trochanteric pain syndrome (GTPS) is the current terminology for what was once called greater trochanteric or subgluteal bursitis. Cortisone injections for GTPS did not provide greater pain relief or reduction in functional limitations than DN. Our data suggest that DN is a noninferior treatment alternative to cortisone injections. Cortisone (corticosteroid) injection into the lateral hip has traditionally been the accepted treatment for this condition; however, the effectiveness of injecting the bursa with steroids is increasingly being questioned.“
- CORTICOSTEROIDS FOR AUTOIMMUNE DISEASES IN GENERAL: Remember that I showed you how these drugs work? They induce immune system suppression, thereby suppressing inflammation which is part of the normal immune system response. At least in theory, this can help slow down the runaway train that is AUTOIMMUNITY. Almost two decades ago, the Australian Prescriber (Corticosteroids in Autoimmune Diseases) gave a great explanation of how these drugs work, along with an important caveat. “How do corticosteroids act in autoimmunity? Corticosteroids induce a transient lymphocytopenia by altering lymphocyte recirculation. They also induce lymphocyte death. The most important immunosuppressive effect of corticosteroids is on T cell activation, by inhibition of cytokine and effect or molecule production. Hazards associated with such therapy are reduced resistance to infection, especially bacterial, and relapse of latent infection such as Herpes simplex and zoster, as well as Pneumocystis carinii and Helicobacter pylori. There is also a risk of acute myocardial ischaemia in pre-disposed patients. Patients on steroids are at increased risk of infection, and symptoms such as fever and pain may be masked by the steroids. Bacterial infections, such as urinary and respiratory infections, are the most common. Corticosteroids accelerate bone loss. Other major adverse effects are aseptic necrosis of bone, psychosis, sleep disturbance, skin fragility and poor wound healing. The eyes should be checked for glaucoma and cataracts.” In the same way that testicles shrink when men take anabolic steroids (because they are taking large amounts of exogenous testosterone-like hormones their testicles’ thermostat-like feedback loop tells their body they already have plenty, thereby shutting down endogenous production), the parts of the brain that make glucocorticoids / corticosteroids (THE HPA-AXIS), shut down endogenous production as well, which the authors of this paper spoke about. “Inhibition of the hypothalamic-pituitary-adrenal axis may lead to adrenal insufficiency when steroids are ceased after long-term use.” It’s easy to find numerous similar studies / warnings from today.
- CORTICOSTEROIDS AND INSULIN RESISTANCE / TYPE II DIABETES: I have shown you that over half the adult American population is believed to have INSULIN RESISTANCE and / or PREDIABETES, with over 10% of the population — including increasing numbers of teens — having full-blown DIABETES. Although there are a mountain of studies linking corticosteroids to one’s propensity to develop Type II Diabetes, I am going to leave you with a very brief overview from Diabetes.co.uk (Corticosteroids and Diabetes). “Use of corticosteroids to treat inflammation can lead to higher than normal blood glucose levels and, in longer term usage may lead to type 2 diabetes developing. One of the side effects of oral corticosteroids is that they can increase blood glucose levels and increase insulin resistance, which can lead to type 2 diabetes. Being on steroids for a longer period of time, over 3 months, may also increase your risk of type 2 diabetes.” Some studies also talked about these steroids increasing the incidence of the various features that characterize PCOS, including hirsutism (women become hairy). PCOS is intimately related to diabetes.
- CORTICOSTEROIDS AND ASTHMA: Because ASTHMA is yet another of the inflammatory diseases that is skyrocketing in incidence with no end in site, there are lots of studies on this topic as well. I’ll show you one from a 2006 issue of the Respiratory Medicine Journal (Systemic Side Effects of Inhaled Corticosteroids in Patients with Asthma). After telling us that, “the presence of chronic inflammation in the airways leads to an increase in recurrent episodes of wheezing, breathlessness, chest tightness, and coughing,” the authors provided a list of some of the potential side effects of steroids, giving well-documented bibliography for each point. “Pharyngitis [sore throat], suppressed HPA-axis function, dysphonia [chronic horseness], adrenal crisis [HERE] cough, suppressed growth velocity in children, bronchospasm, decreased lower-leg length in children, oropharyngeal candidiasis [YEAST INFECTION of the mouth and throat], reduced bone mineral density / bone fractures / osteoporosis [HERE], skin thinning, skin bruising, cataracts, glaucoma.” Another study I found talked about increased incidence of ACNE as well as many others. Notice also that the drugs are causing many of the very problems they are supposed to be helping — a common theme with many medications. Speaking of acne…..
- CORTICOSTEROIDS FOR SKIN CONDITIONS: A study from April’s issue of the Journal of Dermatology (High Rate of Systemic Corticosteroid Prescription Among Outpatient Visits for Psoriasis) provided a microcosm of the entire problem, and not just related to skin conditions. “The use of systemic corticosteroids for the treatment of psoriasis is not recommended according to textbooks and guidelines. In clinical practice, however, many physicians frequently prescribe SC for patients with psoriasis.” This is why I have said repeatedly that when it comes to MEDICAL GUIDELINES, it seems that many are not being followed, and way too many drugs are being prescribed “OFF LABEL“. MY BROTHER, an ER physician, has told me on more than one occasion that using corticosteroid creams is a slippery slope that rarely solves the problem, instead, often leading to the need for more steroid cream. You can read online that this has become an epidemic in some nations. You can also see this same phenomenon when using steroid nasal sprays such as Flonase.
- CORTICOSTEROIDS FOR YOUR DOG: Because there was so much information on the subject, and because our physiology is similar, I am going to include a list of side effects provided by veterinarian Earnest Ward (Steroid Treatment – Long-Term Effects in Dogs) concerning MAN’S BEST FRIEND. “Urinary Tract Infections (UTI), thin skin, blackheads, and a poor or thin hair coat, poor wound healing ability, obesity, muscle weakness secondary to protein catabolism (breakdown), development of hard plaques or spots on the skin called calcinosis cutis, calcium deposition in the skin, increased susceptibility to opportunistic or secondary bacterial infections, increased susceptibility to fungal infections, development of adult onset demodectic mange, diabetes mellitus.” Honestly, it’s pretty much what we’ve seen so far in people.
- OTHER SIDE EFFECTS OF CORTICOSTEROIDS: An article by Kenneth Sagg and Daniel Furst (both MD’s) called Major Side Effects of Systemic Glucocorticoids is a great source for doing more research because they keep an up to date database of studies on the various side effects of these drugs (HERE). When you start suppressing the immune system, it’s like opening Pandora’s Box — especially when you throw the this class of drugs ability to degenerate and deteriorate COLLAGEN-BASED TISSUES.
So why, when we see the crazy number of side effects associated with corticosteroids of every kind (injected, oral, topical), do physicians continue to prescribe them in an almost unbridled fashion for just about everything under the sun? It’s surely not because these drugs are solving the problem — ever. It’s because they are good at relieving pain and symptoms, at least for the short term. But whether taking them for short or long-term, we now know that side effects — many of them quite severe — are almost unavoidable. What’s the solution?
Fortunately, there are any number of ways to address inflammation naturally. The good thing is that I’ve created a generic template that will help many of you — not all, but many — solve your inflammation without dangerous drugs. HERE it is. My gift to you, completely free. An EXIT STRATEGY if you will Not necessarily easy, but simple. Take a look at it and get started today!
