IS ROSACEA PURELY COSMETIC OR A PORTENT OF CHRONIC HEALTH ISSUES?
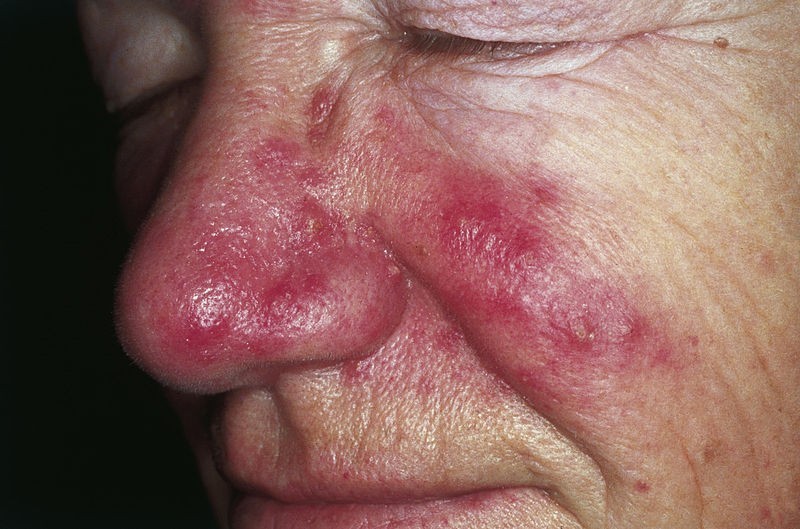
Rosacea. It’s the cherry-red and often times pimply cheeks / nose / forehead / chin, which, according to the National Rosacea Society, affects over 16 million Americans (although some studies put that estimate at almost double that). But what is Rosacea?
Despite the fact that there is a great deal of speculation as to what causes it (we’ll get to that in a moment), the redness and ACNE is at least partially the result of tiny blood vessels on the surface that have dilated. And even though my pics are all of men, not surprisingly, women are much more likely to be affected. One hint as to what causes Rosacea is how it is frequently treated — with antibiotics. Allow me to explain.
Depending on the individual, Rosacea can be triggered by everything from sunlight, to heat, to cold, to certain foods or drinks (alcohol, for instance, is frequently associated with the big red roasceatic nose otherwise known as rhinophyma), to the mites that cause mange, to ENDOCRINE ISSUES, to ROS (free radicals), etc, etc, etc.
However, there are numerous studies associating VARIOUS KINDS OF DYSBIOSIS with Rosacea, one of the most common being something known as SIBO (Small Intestinal Bacterial Overgrowth), which is itself intimately related to IBS (Irritable Bowel Syndrome — recently discovered to be an autoimmune disease).
For instance, back in 2010, the June issue of Clinical Gastroenterology and Hepatology (Increased Incidence of Small Intestinal Bacterial Overgrowth During Proton Pump Inhibitor Therapy) showed that among the several hundred patients studied, “SIBO was detected in 50% of patients using PPIs, 24.5% of patients with IBS, and 6% of healthy control subjects.”
I’ve previously shown you not only how bad PPI’S are for both overall and GUT HEALTH, but I’ve shown you that because they weaken one of the body’s first defenses against microbial invaders (strong stomach acid — see next link), they are heavily associated with H. PYLORI as well. In fact, listen to the conclusions of a study published in the World Journal of Gastroenterology (Extra-Intestinal Manifestations of Helicobacter Pylori: A Concise Review).
“Those of Northern European and Celtic origins appear to be at highest risk of rosacea. It is estimated that the prevalence of rosacea is 1%-10% in fair-skinned populations. Generally, adults over the age of 30 are affected and occurs more often in females. It is thought that inflammation plays a crucial role in its pathogenesis.
Inflammatory mediators from an altered innate immune response leading to generation of reactive oxygen species (ROS) such as nitric oxide appear to be part of the mechanisms of disease. Current evidence most supports extraintestinal manifestations with H. pylori in immune thrombo-cytopenic purpura, iron deficiency anemia, urticaria, Parkinson’s, migraines, and rosacea.”
Although there are a number of bacteria that pop up as potential culprits, research keeps pointing to H. Pylori as the chief pathogen in developing Rosacea. A three month old study from Clinical, Cosmetic and Investigational Dermatology (Rosacea and Helicobacter Pylori: Links and Risks) essentially confirmed this by concluding, “Microorganisms have been addressed in a variety of studies as pathogenic factors. Mite-related bacteria, staphylococcus epidermidis, chlamydia pneumonia, bacterial toxins, and antimicrobial peptide.”
Which brings me to another issue we need to address; what are antimicrobial peptides.
Antimicrobial peptides are simply proteins that have antibiotic properties (MOST PHARMACEUTICAL DRUGS DO AS WELL). While this can be a good thing in the case of peptides, if these proteins get out of balance in your body, they cause dysbiosis. A great example is found in a study from a decade old issue of Nature Medicine (Increased Serine Protease Activity and Cathelicidin Promotes Skin Inflammation in Rosacea).
In this study it was noted that, “Acne rosacea is an inflammatory skin disease that affects 3% of the US population over 30 years of age and is characterized by… the release of cathelicidin antimicrobial peptides. Here we show that individuals with rosacea express abnormally high levels of cathelicidin in their facial skin and that the proteolytically processed forms of cathelicidin peptides found in rosacea are different from those present in normal individuals.“
What studies have repeatedly shown is that individuals with rosacea, SIBO, IBS, and other gut-related problems have something in common as far as treatment is concerned —- antibiotic therapy frequently resolves their problem. In fact, I addressed this in my last post on FMT (Fecal Microbiota Transplants).
The problem is that while antibiotics might be viable for the short term (as long as you are serious about following up with a Gut Health Restorative Protocol — HERE); over the long haul, if there are no lifestyle changes made, the ANTIBIOTICS WILL MAKE PEOPLE WORSE! 100% of the time. Why? Because when you take antibiotics, you destroy the bacteria that live in your Gut (there’s no way around it).
This means that you are destroying as much as 80% of your immune system (HERE). Speaking of immune systems, let’s briefly look at a study that got a lot of play in the press last year as far as connecting the dots concerning the Rosacea / immune system relationship.
A group of Danish researchers looked at the link between Rosacea and a number of CHRONIC INFLAMMATORY DEGENERATIVE and AUTOIMMUNE DISEASES in over 40,000 patients, almost 2/3 of which were women. What did they find? According to results published in the Journal of the American Academy of Dermatology (Clustering of Autoimmune Diseases in Patients with Rosacea)…
“Rosacea is a common inflammatory skin condition that shares genetic risk loci with autoimmune diseases such as type 1 diabetes and celiac disease. Rosacea is associated with type 1 diabetes, celiac disease, multiple sclerosis, and rheumatoid arthritis, in women.”
Having Rosacea doubled the chances of these autoimmune diseases (CELIAC, RA, MS, and T1D).
Besides dealing with underlying INFLAMMATION by addressing Gut Health issues (see earlier links), one interesting Rosacea treatment that I saw come up in the research literature a number of times was LOW LEVEL LASER THERAPY. For instance, September’s issue of the International Journal of Women’s Dermatology (Laser Treatment of Medical Skin Disease in Women) revealed that…
“There are four types of rosacea: erythematotelangiectatic, papulopustular, phymatous, and ocular. Patients may have one or any combination of these types. In the arsenal of treatment for dermatologists, lasers offer a safe and efficacious way to treat some forms of rosacea.”
There were any number of similar studies specifically touting laser treatment of Rosacea.
Bottom line; you need to deal with Rosacea like you would deal with any number of other health-related issues — including autoimmune and inflammatory issues. Firstly, remove the triggers that drive the inflammation. Although there are potentially a slew of them; knowing about the intimate relationship between GRAINS and autoimmunity immediately brings gluten to mind (HERE).
Secondly, address the lesions themselves with a laser (this is an arena where whoever treats you will have to be very careful around the eyes). While Laser Therapy will not likely solve the long-term underlying causes of the Rosacea, it will likely allow for rapid improvement in its appearance — a huge morale booster since this disease affects the face. Thirdly, get with the program as far as Gut Health is concerned (and take a closer look at the relationship between GUT HEALTH AND SKIN).
Also, it’s important to be aware that dysbiosis is almost always associated with some form of “THE LEAKIES“.
