CHRONIC NECK PAIN: WHAT DOES THE LATEST SCIENTIFIC LITERATURE SAY?
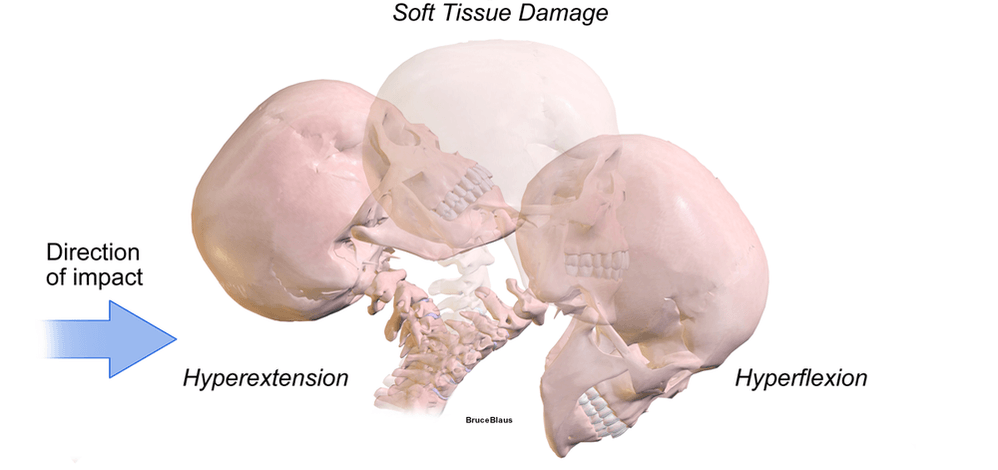
The statistics on WHIPLASH are frightening. As you’ll see again today, study after study show that 50% of those injured in a whiplash-type accident end up with chronic WAD — Whiplash Associated Disorders — pain and dysfunction that never completely go away. The majority of this group not only have CHRONIC NECK PAIN, but as often as not, a host of “bizarre and seemingly unrelated symptoms.”
With something like three million whiplash-type accidents in the US each year, you can see why it’s no wonder that this issue is costing billions upon billions of dollars annually. Although I’ve given you a great deal of information concerning whiplash in the past (click the links above), today I’ll provide a quick look at the current scientific literature on the subject.
- WHAT’S IT LIKE TO LIVE WITH CHRONIC WHIPLASH (WAD)? A month ago, researchers for BMC Musculoskeletal Disorders (Living with Ongoing Whiplash Associated Disorders: A Qualitative Study of Individual Perceptions and Experiences) talked about what it’s like to live with chronic whiplash. “Whiplash associated disorders (WAD) are the most common non-hospitalized injury resulting from a motor vehicle crash. Over the past few decades, recovery rates have remained unchanged with approximately 50% of individuals experiencing on-going pain and disability. Results from intervention trials for individuals with chronic WAD are equivocal and optimal treatment continues to be a challenge. ll participants described navigating the healthcare system after their whiplash injury to help understand their injury and interpret therapeutic recommendations. Participants highlighted the need to find the right healthcare practitioner to help with this process. Many participants also described additional complexities in navigating and understanding healthcare incurred by interactions with compensation and funding systems. Participants in this study had been living with WAD for an average of 6.5 years and continued to find it challenging and exhausting.” It’s called the MEDICAL MERRY-GO-ROUND folks, and unfortunately, it’s dog common to watch people going round and round until it literally destroys them. One of the situations that these authors spoke of was the reluctance of doctors to believe these patients, instead, seeing it as a ploy for a legal / financial settlement, or getting their disability.
- WHIPLASH / WAD SCREWS UP THE BRAIN: In the brain and spinal cord, the gray matter is the inner portion, where most of the nervous system’s chief functions take place. The white matter (it’s white because it’s cells are covered by a fatty substance called myelin) is made up of cells that connect the gray areas to each other. Although there are numerous studies showing that whiplash affects the brain, this month’s issue of Human Brain Mapping (Differences in White Matter Structure and Cortical Thickness Between Patients with Traumatic and Idiopathic Chronic Neck Pain: Associations with Cognition and Pain Modulation?), concluded that, “Cortical thinning in the left precuneus was revealed in WAD compared with CNP (chronic neck pain) patients. The extent of white matter structural deficits in the left tapetum coincided with decreased conditioned pain modulation efficacy in the WAD group. This yields evidence for associations between decreased endogenous pain inhibition, and the degree of regional white matter deficits in WAD.” Thin the precuneus and you’ll end up with memory, visuo-spatial processing, and self consciousness issues. The tapetum is important because it’s associated with the Corpus Collosum — the connection between the brain’s two hemispheres. Mess with the tapetum and the two sides cannot communicate properly.
- WAD & NECK PAIN BOTH CAUSE IMPAIRMENT OF MOTOR FUNCTIONS: When there is enough damage to the brain, not only does this affect the sensory side of the brain (PAIN, paresthesias, LOSS OF PROPRIOCEPTION, etc), but it’s becoming increasingly clear that it affects the motor side of the brain as well. The journal Spine (Motor Impairment in Patients with Chronic Neck Pain: Does the Traumatic Event Play a Significant Role?) recently concluded that, “Motor impairment was observed in both patient groups (CNP & WAD) with a higher degree in patients with chronic WAD. These impairments were linked to self-reported disability and were in most cases associated with pain, fear-avoidance, and symptoms of central sensitization.” Click the link if you are not sure what CENTRAL SENSITIZATION is. This was confirmed visually (DIAGNOSTIC ULTRASOUND) in a study published in the American Journal of Physical Medicine & Rehabilitation (Alterations in the Mechanical Response of Deep Dorsal Neck Muscles in Individuals Experiencing Whiplash-Associated Disorders Compared to Healthy Controls: An Ultrasound Study), which concluded that “the mechanical responses of the deep dorsal neck muscles differ between individuals with WAD and healthy controls, possibly reflecting that these muscles use altered strategies while performing a neck extension task.” Just realize that when you start down the road of ALTERED SPINAL / FASCIAL BIOMECHANICS, degenerative arthritis isn’t far behind.
- WAD TURNS NECK MUSCLES TO FAT: Although we’ve known about this phenomenon in the low back for decades (THORACOLUMBAR AREA), not surprisingly, the same thing occurs in necks. After comparing “Thirty-one subjects with WAD and 31 age and sex matched controls, twenty-one (68%) patients had mild/moderate disability and 10 (32%) were considered severe. Statistically significant differences in regional MFI (Muscle Fatty Inflitration) were particularly notable between the severe WAD group and healthy controls.” This study was found in the journal Spine (The Qualitative Grading of Muscle Fat Infiltration in Whiplash Using Fat/Water Magnetic Resonance Imaging) and is why strength training is so critical, not just for chronic neck pain, but in general.
- PREDICTING WHO’S GOING TO GET OVER THEIR WAD: As I have shown you in the past, predicting who is going to improve after having a whiplash injury is difficult to determine, although there are a few things we know — women and the elderly almost universally have a much tougher row to hoe than young, healthy, males. Just days ago, the journal Spine (The Potential and Perils of Prognosticating Persistent Post-Traumatic Problems from a Post-Positivist Perspective) stated that, “Predicting recovery following traumatic neck pain has become an active area of research but is moving in several different directions with currently little consensus on the important outcomes to predict or relevant variables to predict them.” The Journal of Physiotherapy confirmed this with a paper that reviewed 46 studies of 99 models used to predict whiplash severity and subsequent improvement. The study’s title tells the story, Few Promising Multivariable Prognostic Models Exist for Recovery of People with Non-Specific Neck Pain in Musculoskeletal Primary Care: A Systematic Review.
- WHAT IS THE MEDICAL COMMUNITY DOING ABOUT WAD? Not to sound harsh, but who do you think brought us the opioid epidemic? (Doctors were not the sole culprits; THE GOVERNMENT was in on this as well.) In this vein, we can’t be shocked that THE BIG FIVE still rules the day (along with a round-robin of ever-changing novelties). A few weeks ago the journal BMC Musculoskeletal Disorders published a study called Management of Whiplash Associated Disorders in Australian General Practice that stated, “Whiplash Associated Disorders (WAD) are common and costly, and are usually managed initially by general practitioners (GPs). Motor Vehicle Crashes (MVCs) are the cause of 50 million injuries worldwide and nearly four million emergency department (ED) consultations annually in the US. After being medically evaluated, approximately 90% of those who present to ED after MVC return home. Only around 50% of those with WAD will fully recover, with 30% remaining moderately to severely disabled, creating significant personal, economic, and social distress. Worldwide, chronic pain following MVC is a significant burden and a frequent and expensive public health problem. Current clinical guidelines recommend that the most important aspect of management of acute WAD is providing assurance and encouragement to return to normal activities and exercise, but GP provided advice/education was only documented in 5.8 per 100 WAD problems in our study. Local injections, muscle relaxants, anti-convulsants, benzodiazepines and anti-depressants, for which there is no evidence for efficacy and which are not recommended, were overused. Non-recommended treatments were used in a total of 34.4 per 100 WAD cases.“
- WHAT IS THE MEDICAL COMMUNITY DOING ABOUT CHRONIC WHIPLASH PART II? LYRICA is a terrible drug (not my opinion, but verified by studies and the majority of those who have tried it). It is essentially second generation Neurontin (gabapentin) — one of the FOUR DRUGS that Pfizer was fined 2.3 billion dollars for promoting “OFF LABEL” (they were fined 430 million dollars for the same thing with Neurontin itself). Just last week, Australian officials announced plans for a study to see if Lyrica could prevent chronic whiplash / WAD if given in a prophylactic manner in the ER, post-accident (Pregabalin Versus Placebo in Targeting Pro-Nociceptive Mechanisms to Prevent Chronic Pain After Whiplash Injury in At-Risk Individuals – A Feasibility Study…).
WHAT’S BEING DONE TO SOLVE CHRONIC WHIPLASH PAIN (WAD)?
As you have already seen, despite a myriad of things that have been tried to alleviate chronic WAD, sure-fire solutions remain elusive. Or as one study above stated, “equivocal“. What does equivocal really mean? Merriam-Webster defines it thusly, “Subject to two or more interpretations and usually used to mislead or confuse. Uncertain as an indication or sign. Of uncertain nature or classification. Of doubtful advantage, genuineness, or moral rectitude.”
The results aren’t negative, but they aren’t positive either. It’s a wash. Doesn’t exactly inspire confidence, does it? But are there new treatments showing promise for those struggling with chronic WAD / whiplash? Although we could debate the definition of the word “promise” for decades, here are some things from the past few weeks that at least according to the research, could prove beneficial.
- THE RIGHT KIND OF PATIENT EDUCATION: One thing we are seeing again and again in peer-review is the need for quality patient education (by “patient education” I do not mean trying to convince patients they will require MASS QUANTITIES OF ADJUSTMENTS). In a Disability and Rehabilitation study from a year ago (What Information do Patients Need Following a Whiplash Injury? The Perspectives of Patients and Physiotherapists), the consensus seemed to be that those with WAD need to be reassured as well as educated. “Reassurance can be an effective communication tool to decrease patients concerns about their injury and help strengthen the patient-health practitioner relationship. Although clinical guidelines for the management of whiplash injuries recommend that individuals must remain physically active post-injury, statements from the patient group indicate that this information is not always provided and clearly explained to patients.” A brand new study from Physiotherapy Theory and Practice (The Effects of Pain Neuroscience Education and Exercise on Pain, Muscle Endurance, Catastrophizing and Anxiety in Adolescents with Chronic Idiopathic Neck Pain) talked about the need for both pain neuroscience education (PNE) and exercises for those with chronic neck pain. What is PNE? It’s essentially explaining to patients that their pain may no longer be arising from damaged tissue, but might be coming from the brain itself. In other words, the pain may have become “centralized” (CENTRAL SENSITIZATION), which is never a good thing.
- EXERCISES PLUS MOBILIZATION / MANIPULATION IS BETTER THAN EITHER ONE ALONE: Yet another study (The Effects of Neck Mobilization in Patients with Chronic Neck Pain), this one from Monday’s issue of the Journal of Bodywork and Movement Therapies, provided evidence to this thought process. Stick around and in just a moment I will show you why ADJUSTMENTS work like magic for many sufferers of WAD — but only under certain specific circumstances.
- DIRECTION-MOVEMENT CONTROL TRAINING MAY PROVE EFFECTIVE FOR CHRONIC NECK PAIN: It’s unsettling when a journal (in this case, this month’s issue of the Journal of Bodywork and Movement Therapies) makes this sort of statement. “There is low level evidence that cervical interventions are effective on pain and range of motion at the immediate follow up, but no evidence on the effectiveness of the direction movement control intervention especially on the effectiveness of long term follow up.” The study (Long-Term Effect of Direction-Movement Control Training on Female Patients with Chronic Neck Pain) concluded, however, that “Direction-movement control training is likely to be an effective training program to enhance body functionality through improvement of pain, function, endurance, head repositioning accuracy, range of motion, and cervical flexor endurance.” If you want to see what Direction-Movement Control Training looks like, the study is free online.
- PILATES FOR CHRONIC NECK PAIN: Earlier this week, the same journal published yet another study on chronic neck pain (Is Pilates an Effective Rehabilitation Tool? A Systematic Review) showing that after reviewing 23 studies on the subject, “The majority of the clinical trials in the last five years into the use of Pilates as a rehabilitation tool have found it to be effective in achieving desired outcomes, particularly in the area of reducing pain and disability.” I’ve shown you in the past that the same thing is true of yoga.
What kind of conclusions can we make from this mish mash of research? I’m honestly not quite sure. As the very first study discussed stated, part of the process is about each individual figuring out their own unique situation and what works for them.
“A process of trial and error by participants was used to identify suitable strategies. Specific but different strategies were employed to prevent pain or to alleviate pain. Establishing these strategies took time, and several participants felt that an early lack of awareness of the potential for on-going pain led them to underestimate the importance of early management and ultimately contributed to their chronic condition. Individuals with acute WAD have also expressed a desire for more realistic expectations of recovery.”
What makes it so darn difficult is that when it comes to the tests, you’re not likeely to have anything to show for them (all tests and imaging are usually normal / negative after whiplash-like injuries; even the more serious ones).
My opinion, especially when it comes to those dealing with chronic or long-term WAD, is that there are frequently some missing links. One of these is dealing with SYSTEMIC INFLAMMATION. And related to it, dealing with SCAR TISSUE as well (inflammation always leads to formation of scar tissue that the medical community refers to as “fibrosis” — HERE).
As I wrote about a couple of years ago, the first step in solving chronic neck pain is to restore normal cervical range of motion (HERE), which must involve both sectional and segmental motion of the neck (HERE). These points provide the basis for PHASE I and PHASE II of effectively addressing chronic neck pain and/or issues related to WAD.
Bear in mind that when I talk about dealing with inflammation, I am not simply talking about (as is usually the case with the medical community) making sure you have plenty of the “BIG FIVE” class of drugs on hand. I am talking about the need to effectively deal with whole body inflammation that can arise from numerous sources and be magnified by the effects of the WAD. To get a better idea of what I mean, take a look at THIS POST. And be sure to like, share or follow on FACEBOOK while you are at it!
