OSGOOD SCHLATTER SYNDROME
Osgood Schlatter’s Syndrome is as painful as it is common. And make no mistake, it is common — without doubt the most common form of chronic knee pain in children, adolescents, and excepting PATELLAR-FEMORAL SYNDROME, possibly even young adults. It is a form of TENDINOPATHY that is frequently characterized by a painful, swollen, knot (an “avulsion”), an inch or so below the knee cap. This knot is typically hyper-sensitive and is aggravated by physical activity or getting it bumped. People who have struggled with Osgood Schlatter will tell you that even a small bump to the tubercle can create the sort of pain that can make one pass out.
MORE OSGOOD SCHLATTER SYNDROME
(Chronic Knee Pain in Children & Adolescents) Osgood Schlatter is found mostly in adolescents or teens that have either played organized youth sports, or have undergone a major growth spurt, and is frequently associated with microscopic FASCIAL ADHESIONS of the muscles in a very specific area of the leg. Typically, these adhesions occur because of overuse and abuse, and / or muscle imbalance — the front thigh muscles (Quadriceps) are naturally much stronger than the muscles on the back of the thigh(Hamstrings), and sports tend to compound this imbalance. Many young people end up quitting sports or curtailing their physical activity because of the incredible pain involved with Osgood Schlatter Syndrome and the inability of standard medical therapies to solve the problem. There are three main reasons that standard medical approaches often fail.
- TREATMENT IS BASED ON PRESCRIPTION: Not only are PAIN MEDS, MUSCLE RELAXERS, NSAIDS, and CORTICOSTEROIDS, ineffective for Osgood Schlatter’s Syndrome, but they can be dangerous as well. The problem is that far too many doctors are using a treatment model that is based on ‘itis‘ (INFLAMMATION) instead of ‘osis‘ (the tissue derangement I refer to in my office as “SCAR TISSUE” and the medical community calls “FIBROSIS“). It is a model that was scientifically outdated three decades ago! Anti-inflammatory drugs of all kinds degenerate collagen-based connective tissues (as do CERTAIN KINDS OF ANTIBIOTICS), and lead to kidney, liver, and heart problems with prolonged use as well. Remember the old slogan, “Tylenol… Nothing Safer “? THEY LIED.
- TREATMENT IS OFTEN AIMED AT THE WRONG AREA: Treatment is frequently focused on the painful tibial tubercle below the knee instead of focusing on the real source of the problem (hint; the Scar Tissue / Fibrosis). Several years ago I treated a college basketball player from a local town (he was a junior or senior at the time). He had been receiving treatment (sometimes hours a day) since the 8th grade — all at the painful Tibial Tubercle. I found the FASCIAL ADHESION, broke it up, and he was 90% better — instantly (HERE)! Sometimes the problem is at the tubercle itself; usually it’s not.
- TREATMENT DOES NOT INCLUDE BREAKING SCAR TISSUE: Osgood Schlatter’s Syndrome is typically addressed by resting and doing lots of stretches. A nice thought……. But until the restricting adhesion is dealt with, rest and stretching are usually (in all but the most minor cases) ineffective. And let’s face facts. How many athletes want ‘prolonged rest’ as part of their regimen?
OSGOOD SCHLATTER SYNDROME AND ITS
RELATIONSHIP TO THE KNEE JOINT
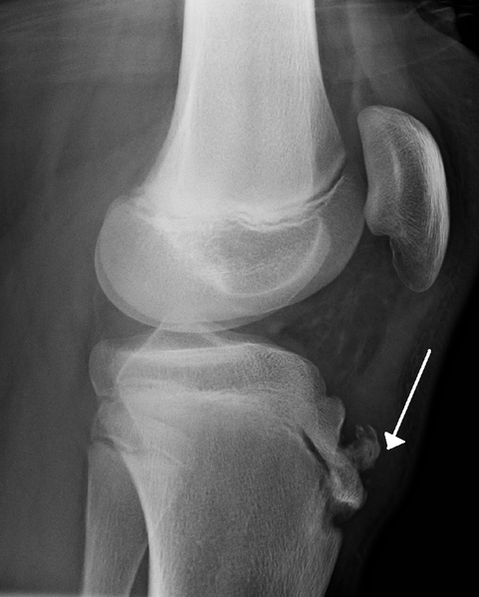
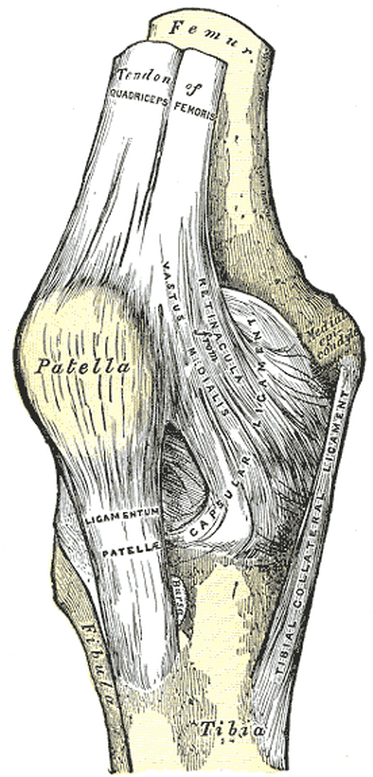
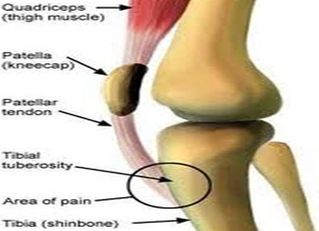
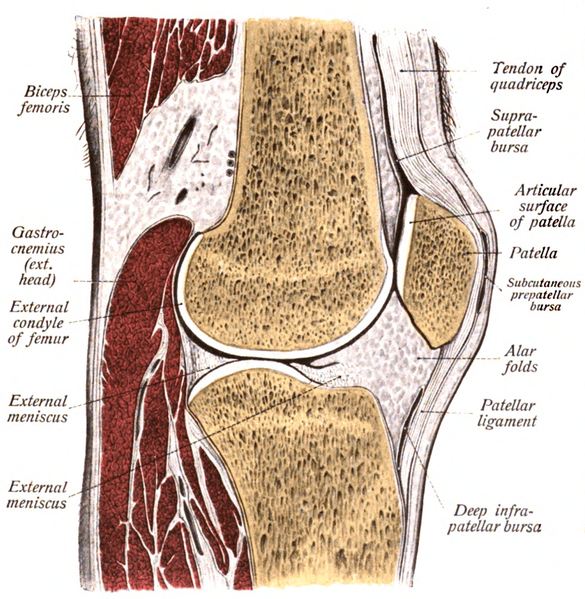
The short (one inch) Patellar Tendon found just blow the knee cap anchors to the top of the shin bone and creates a small bony “bump” called the Tibial Tubercle (circled in top right). One of the rules of Anatomy & Physiology (Wolff’s Law) states that, “Bone grows in response to mechanical stress, whether that stress is good or bad“. With Osgood Schlatter Syndrome, the small bump that is the normal Tibial Tubercle has so much mechanical pressure put on it begins to avulse the periostium away from the bone itself, while the calcium laid down in response becomes a bony knob — a knob that can cause excruciating (even crippling) pain when bumped or hit.
Dr. Schierling’s protocol for treating Osgood Schlatter Syndrome utilizes techniques similar to those used by the physicians and clinicians that treat both professional and college sports teams. In most cases, it takes just one or two in-office treatments to see a major change, and it is not uncommon to see a dramatic change immediately upon treatment. Patients are then given simple stretching and strengthening programs to do at home in order to restore the strength, balance, and mobility to the knee.In over fifteen years of treating people with Osgood Schlatter Syndrome using these specific protocols, I am not sure that I have ever failed to see a case resolve or at least dramatically improve.