THORACOLUMBAR-DRIVEN LEG PAIN / SCIATICA: IS IT A REAL THING? LET’S ASK THE SUPERIOR CLUNEAL NERVE
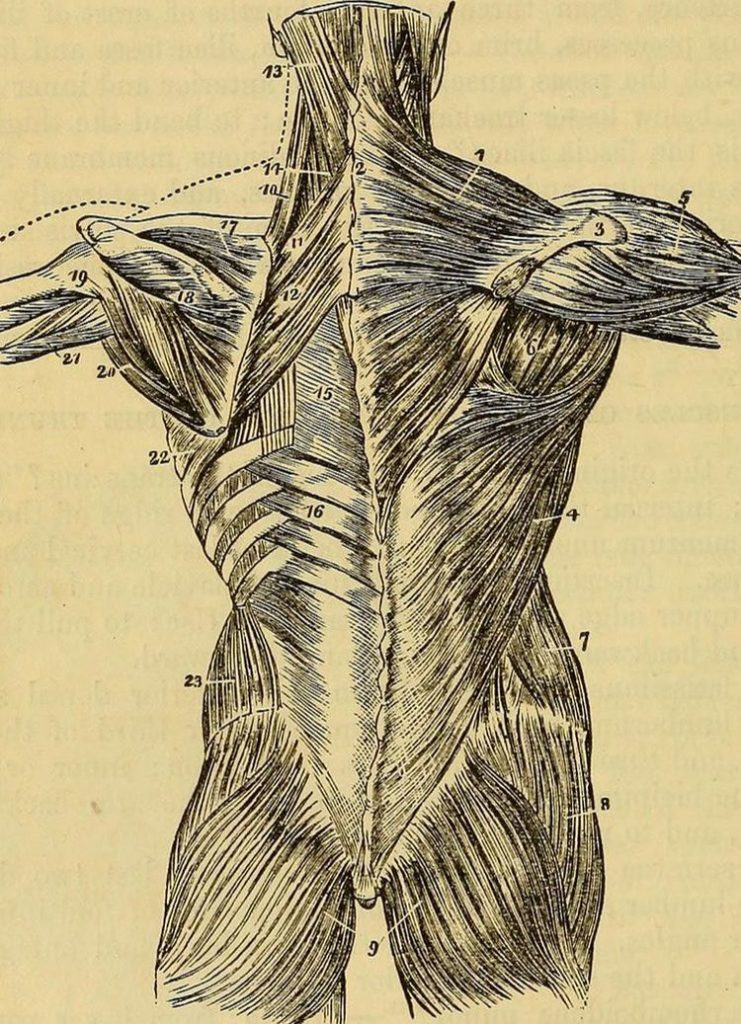
Almost two decades ago I realized that low back pain was often times the result of problems in the Thoracolumbar Fascia (HERE, HERE and HERE). Not long after, I learned that as much as a third or more of SCIATICA (leg pain) is the result of PIRIFORMIS SYNDROME. What if I told you that evidence is increasingly pointing to FASCIAL ADHESIONS as a major culprit in sciatica as well?
This is exactly what last month’s issue of the Journal of Pain Research (Anatomical Etiology of ‘Pseudo-Sciatica’ From Superior Cluneal Nerve Entrapment: A Laboratory Investigation) concluded. The study, done by eight orthos, neuros, and anatomists, from Tokyo University revealed that…..
Low back pain (LBP) is a common condition with a life-time prevalence affecting up to 84% of the population. Chronic LBP is less prevalent, occurring in about 23%. Large epidemiological studies have shown that up to 37% of patients with chronic back pain have a neuropathic pain component, mainly presenting as radicular [radiating] leg pain.
The authors go on to talk about a number of studies showing how this leg pain is frequently not a true sciatica, but instead a “pseudo-sciatica” caused not by irritation of the nerve roots themselves, but by irritation / entrapment of a cutaneous or superficial nerve known as the Superior Cluneal Nerve (SCN).
As you will see in the pictures below, the SCN travels in the superficial layer of the Thoracolumbar Fascia (you can actually see these layers moving independently of each other HERE with the proper technology) just above the posterior portion of the illiac crest — the large bones just below the bottom of the ribs that you use when you put your hands on your hips — before popping through said fascia and supplying feeling to the upper half of the buttock.
PICTURES OF A RIGHT BUTTOCK / HIP AND A RIGHT BUTTOCK PIRIFORMIS MUSCLE
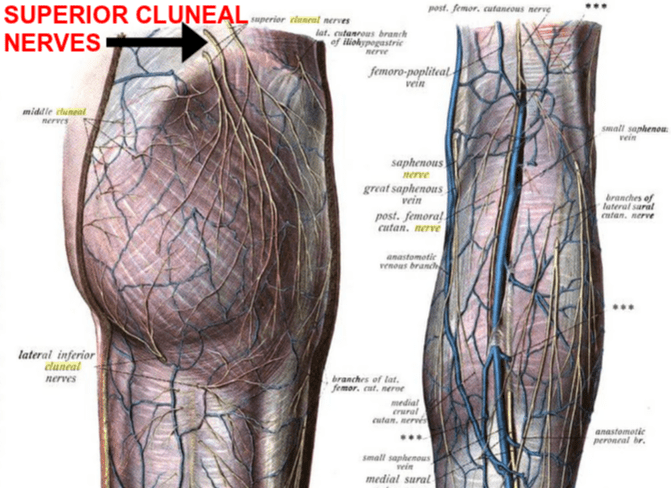 | 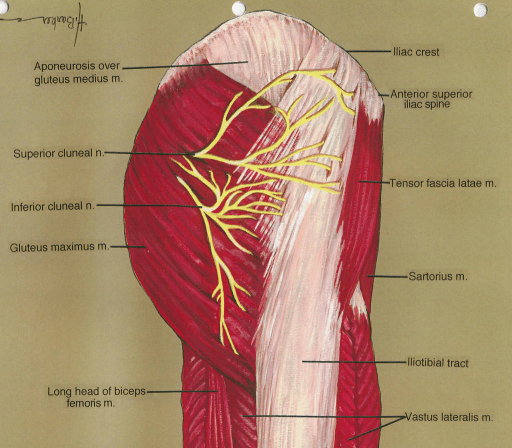 |
Firstly, notice how there is a layer of FASCIA covering everything in the picture on the left. Now notice the arrow at the top showing the three branches of the SCN piercing the fascia that makes up the osteofibrous tunnel (it’s the medial or “middle” branch that is the most commonly entrapped). The picture on the right is labeled incorrectly. It actually shows the middle cluneal nerves and not the SCN. This begs the question; can the MCN likewise become entrapped?
A 2016 issue of the World Journal of Orthopedics — Entrapment of Middle Cluneal Nerves as an Unknown Cause of Low Back Pain — stated that, “Entrapment of middle cluneal nerves induces low back pain and leg symptoms… and is possibly an under-diagnosed cause of low-back and/or leg symptoms.” In the picture on the right, the Superior Cluneal Nerves would actually be coming through the fascia at the area where the white dot is at (middle top).
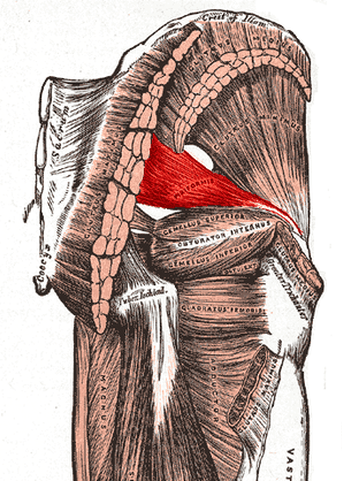
I included the pics below simply because of their proximity to the PIRIFORMIS MUSCLE (they overlay it superficially). These pics also show the illiac crest (the large curved ridge of bone) that the gluteal muscles originate from. I have thought for a long time that some of what I have historically called Piriformis Syndrome is actually entrapment of the SCN.
 | 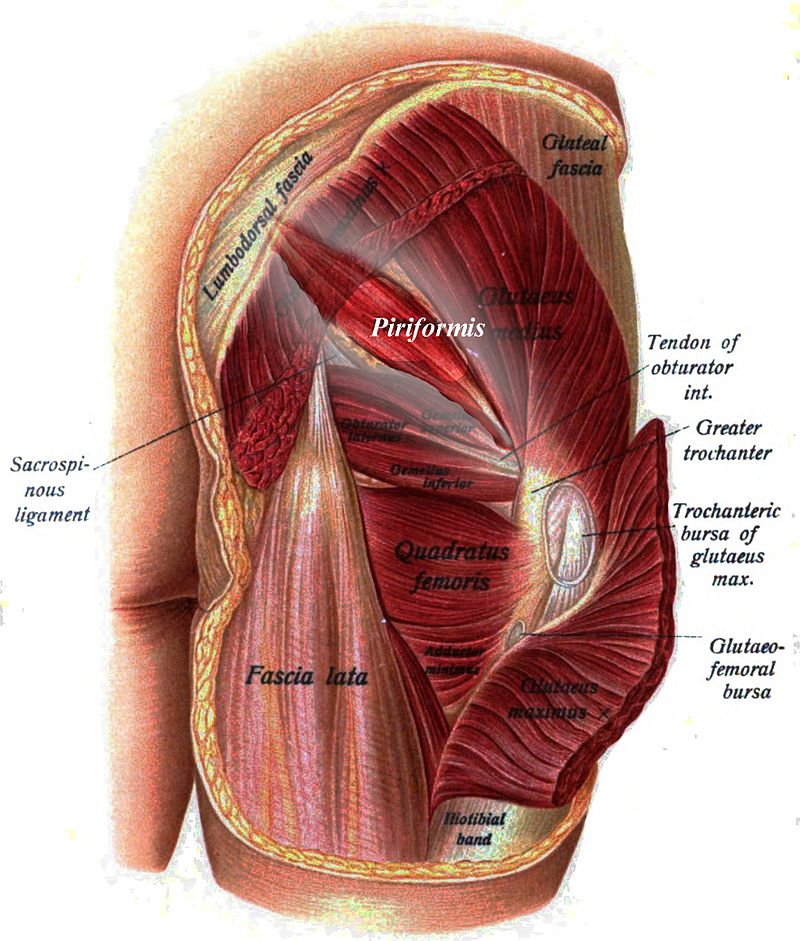 |
It’s super easy to assume that pain in the area we have been discussing is caused by the usual suspects — a DISC ISSUE, PIRIFORMIS SYNDROME, or a SACROILIAC PROBLEM. There’s another problem I am leaving out — something called Thoracolumbar Junction Syndrome or Maigne’s Syndrome (named after a French surgeon). This occurs when SUBLUXATION of the spinal area where the ribs end (T-12) and the lumbar spine begins (L-1) refers pain to the very area we’ve been discussing, as well as the groin, the lower abdomen, the sex organs (testicles / ovaries), and the upper portion of the IT-BAND.
This is why tightness in the Thoracolumbar area of the spine is often times not simply a compensation for what’s going below it at the lumbosacral area; it’s frequently itself the primary problem. The obvious connection here is that the Superior Cluneal Nerves arise from the spinal levels (T-12, L-1, and L-2) otherwise known as the Thoracolumbar spine.
What’s crazy is that just as there are experts telling us that the number one cause of buttock pain and sciatica is problems with the Piriformis, I likewise found people touting Superior Cluneal Nerve Entrapment as the number one cause of both as well. Which begs yet another question; can SCN Entrapment be imaged? A group of scientists and researchers from the neurology department at Austria’s Medical University of Vienna published a paper (Successful Identification and Assessment of the Superior Cluneal Nerves with High-Resolution Sonography) in a recent issue of the journal Pain Physician saying yes.
“We hereby confirm that it is possible to visualize the medial branch of the superior cluneal nerves (mSCN) in the majority of anatomical specimens. The patients described may indicate a higher incidence of mSCN syndrome than has been recognized. mSCN syndrome should be considered in patients with low back pain of unknown origin.”
The problem is that while this technology clearly shows the fascial layers either moving normally or restricted in their movement (HERE), it is not yet in common use (meaning that in most cases, insurances will not cover it).
The real question now that you’ve been diagnosed a Cluneal Nerve Entrapment is how to go about having it treated? Although the medical literature is replete with information on nerve blocks, NSAIDS, CORTICOSTEROID INJECTIONS, and a wide variety of surgical procedures (usually in the form of fascial releases), I use a combination of adjustments (frequently focusing on the Thoracolumbar Junction) as well as TISSUE REMODELING and LLLT.
Because in most cases this is a fascia issue, there are many who have good results with ACUPUNCTURE as well as DRY NEEDLING. While a conservative approach does not always work, drugs are never a long-term solution. And honestly; why would you want to start with surgery anyway?
This thought process was driven home by a Japanese study published this past July in the journal Spine Surgery and Related Research (Treatment of Low Back Pain Elicited by Superior Cluneal Nerve Entrapment Neuropathy After Lumbar Fusion Surgery). In this study, the authors took individuals who had undergone lumbar spinal fusion (you know, pins, screws, rods, wires, STABILIZERS, etc), yet still struggled with pain and sciatica (here in America we refer to this as Failed Back Surgery Syndrome).
The authors then did a Trigger Point Injection at the area where the Superior Cluneal Nerve exits the Thoracolumbar Fascia (see earlier pic with arrow at top) to see if it would help. 75% had relief (but since the relief was short-lived, release surgery was done on the osteofibrous tunnel).
Stay tuned because my NEXT POST is going to be on Cutaneous Nerve Entrapments in general. That’s right; these sorts of entrapments can happen all over the body, causing a myriad of chronic pain issues that are rarely solved simply because they are rarely addressed, let alone looked for. Oh; and make sure to check out the cool video below by Dr. Rick Boatwright, an Arizona DC who has written extensively about why he believes SCN Entrapment is the number one cause of low back pain / sciatica (pseudo sciatica) facing our population today.
If you are one of the millions of Americans struggling with Low Back Pain, make sure to read my DIY article for getting rid of yours (HERE). While you’re at it, make sure to spread the wealth by liking, sharing, or following on FACEBOOK. It’s the easiest way to reach those you love and care about most with potentially life-changing information.
