ROME’S DR. BRUNO BORDONI; EXPERT ON FASCIA AND IT’S RELATIONSHIP TO PAIN, DYSFUNCTION, AND DISEASE

Although first touted by DR ANDREW TAYLOR STILL, there is a growing number of elite scientists researchers, and physicians, who believe the solution to many — some would say most — chronic illness and chronic pain is in the fascia (HERE). We could definitely add one more to this list; Italy’s Bruno Bordoni.
Dr. Bordoni (a physician, physical therapist, professor, and researcher at Rome’s TorVergata University and Milan’s Don Carlo Gnocchi Foundation) is in rarefied air when it comes to researching fascia. Today I want to briefly take you through some of his studies on FASCIA, showing you how it really is related to everything that goes on in the body (for the record, many of Bordoni’s studies are co-authored by Dr. Emiliano Zanier — another Italian).
The first study we’ll discuss today is from a 2014 issue of the Journal of Multidisciplinary Healthcare (Clinical and Symptomatological Reflections: The Fascial System), The authors, Drs. B & Z, reveal that “Every body structure is wrapped in connective tissue, or fascia, creating a structural continuity that gives form and function to every tissue and organ. The human body must be considered as a functional unit, where every area is in communication with another through the fascial continuum, consequently originating perfect tensegritive equilibrium.”
Right away the authors reveal that fascia is not only a mechanical continuum / structural continuum (TENSEGRITY), but is intimately involved in communication as well (FASCIA IS ITS OWN NERVOUS SYSTEM).
They went on to talk about the importance of both fibroblasts (which we will discuss later) and the ECM (fascia’s “gelatinous substance known as extracellular matrix, where numerous molecules (ie, glycosaminoglycans, proteoglycans and polysaccharides such as hyaluronic acid) can be found“). They then discussed the way that the layers of fascia glide on each other (“The superficial fascia is made up of different layers, whose formation facilitates the sliding of one layer over another“).
If you want to see what this looks like, one of the coolest things on my site is THIS TWO PARAGRAPH POST showing a side-by-side comparison (10 second videos) of the difference in the gliding ability of the low back fascia of people with low back pain, and people without.
For those of you fascinated by fascia as related to the LYMPHATICS, “according to some texts, within the superficial fascia there is a vascular network independent of the lymphatic and blood pathways. It is called the Bonghan duct system.” This is part of what allows fascia to act not only in a physical and neurological manner, but in a neurochemical manner as well — it actually acts as a separate endocrine system (HERE). Furthermore, fascia is its own PROPRIOCEPTIVE SYSTEM as well, likely containing as much proprioceptive power as any other single tissue.
“The deep fascia is the last connective layer before coming in contact with bones, muscles, and the visceral [organs], and vascular systems. Its vascular and lymphatic system is well developed, with numerous corpuscles in charge of proprioception…. The fascial continuum can be considered a sense organ of human mechanics….”
When proprioceptors / mechanoreceptors are not fired off to the brain (the most obvious reason for this would losses of motion, both SECTIONAL & SEGMENTAL), it’s been said that every message that’s prevented from going up to the brain (sensory messages are otherwise known as “afferent“), inhibits thirty responses coming back down on the motor (“efferent“) side. This is at least part of the reason that decreased function of fascia, and the abnormal firing of mechanoreceptors / proprioceptors that follows, is increasingly being associated with various disease states in the peer-reviewed literature.
“The muscle system is part of the fascial continuum, and when it is affected by pathologies or systemic disorders such as visceral [organ], genetic, vascular, metabolic, and alimentary [digestive] disorders, its function undergoes a nonphysiological alteration; there are many epigenetic processes that can lead to its adjustment as a response to mechanotransductive stimuli, resulting in further decrease of its function and properties.
Once altered, the fascial continuum generates a symptomatology that deteriorates the health condition of the patient, very often developing symptoms that are more significant than the clinical parameters diagnosed through medical diagnostic devices. The nociceptive afferent inputs [pain or similar] from the fascial system can modulate the afferent response from the central nervous system.
If the afferent is not physiological, the efferent will be in dysfunction and in pathology. An increased level of circulating cytokines originating in the connective system, due to systemic pathologies, could develop neuropathic pain.”
Pay attention to what this is saying. When MECHANOTRANSDUCTION (the ability to convert mechanical energy into electrical messages) is altered by faulty or “altered” BIOMECHANICS, there is a loss of function that goes far beyond anything we can see with current technology (CT, MRI, X-rays, etc). The symptoms that develop as the result of said biomechanical dysfunction may not only be severe, they are also not nearly as controlled by genetics as they are by “epigenetics” (HERE).
When this cycle gets going, it can become “vicious,” feeding itself. Furthermore, when you add circulating CYTOKINES (INFLAMMATION) to the mix, the result can be the neuropathic pain we refer to as CENTRAL SENSITIZATION (in many of his studis he talks about ALLODYNIA & HYPERALGIA), with the paper’s next several paragraphs talking about fascia’s relationship to “normal” pain. When I say ‘normal’ I mean the everyday chronic, severe, pain that’s caused by SCAR TISSUE (fascia that has become FIBROTIC and THICKENED, or “DENSIFIED“).
“The loss of a correct sliding of the layers is demonstrated by an increased density of the fascial thickness… termed… fascial densification. Defective sliding, for instance due to a scar, generates tension, which then affects the fascial continuum, developing painful symptoms.
Tensional alterations can derive from the contractile property of fibroblasts, creating a fascial tonus that is independent of neurological intervention. A nonphysiological [pathological] mechanical environment stimulates an inflammatory environment, with resultant fibroblasts’ hyperplasia and further fascial densification, which then develops into chronic inflammation and into the sensitization of nociceptors.”
Because I am running out of time, let me give you an overview of the rest of the paper. The authors speak at length about the relationship between OSTEOPOROSIS & INFLAMMATION, saying “The fibroblasts (the foundations of the fascial system) affect the immune system, and as a consequence bone tissue; this phenomenon is called osteoimmunology,” and then going on to mention that the same phenomenon is likely present in RA.
Not surprisingly, they talk about some of the principles mentioned in Meyer’s ANATOMY TRAINS (“The fascial continuum can also develop symptoms in areas which are far from the original dysfunctional point“) as well as discussing CHRONIC NECK PAIN caused by dysfunciton of the CERVICAL FASCIA (“an alteration in the thickness of the fascial layers has been verified, with consequent altered spinal mobility and pain“).
Beyond pain, said dysfunction also causes many of the mechanics of vision to be abnormal, as well as gait and balance issues. The authors end by spending a number of paragraphs showing how fascia is an organ of special senses that have been referred to as “interoception“. Interoception?
FASCIA AND INTEROCEPTION

Mechanoreception, mentioned earlier, deals with your body’s ability to sense “mechanical” entities like stretch, pressure, movement, vibration, etc. Interoception is a bit different. In a study probably not named after Ric Ocasek’s 1986 hit (HERE), last year, Complimentary Medicine Research carried a study called Emotions in Motion that dealt with something known as the Body / Mind (aka the Mind / Body Connection).
Dr. B kicked things off by talking about some of the “pioneers of psychotherapy,” and the way they connected the psyche to the body in a single “mind-body functional unit“. Bordoni went on to talk about the ways that some of the same receptors that sense mechanical activities (the mechanoreceptors that allow for proprioception) have the ability to act in terms of interoception.
While Oxford’s Reference Guide defines ‘interoceptor’ thusly (“any receptor organ composed of sensory nerve cells that respond to and monitor changes within the body, such as the stretching of muscles or the acidity of the blood“), Bordoni himself says…..
Interoception is the awareness of the bodily condition based on the information derived directly from the body. The pathways pertaining to interoception project towards the autonomic and medullar homoeostatic centers and the brainstem, where they are routed to the frontal cingulate cortex and the dorsal posterior insula, by the thalamocortical circuit. Interoception can modulate the exteroceptive representation of the body, as well as pain tolerance; dysregulation of the pathways that manage or stimulate interoception could cause a distortion of one’s own body image, influencing emotionality.
The authors went on to discuss how different kinds of bodyworkers, PT,s chiros, osteopaths, etc, etc, are able to stimulate these areas of the brain by stimulating the interoceptors found in fascia, thereby affecting the body “emotionally“.
They then discussed various pathways and mechanisms, specifically addressing the way that “skeletal muscle tensional load” along with “fascial deformation” (HERE is a link to fascial deformation) are able to increase blood flow via sympathetic response, which triggers certain responses in the brain (“Scientific research has proven that the fascial continuum is innervated by the autonomic sympathetic system“).
This is why HOMEOSTASIS is critical in the autonomic nervous system, and why SYMPATHETIC DOMINANCE can cause problems in the body, the mind, and the emotions. As crazy as it may sound to those within the mainstream, “A disorder involving the myofascial system will have repercussions on the emotional state. There is a strong relationship between the myofascial structure and the emotions.” Bordoni goes on to say…
“We can say that the presence of a disorder of the myofascial continuum, during everyday movements and activities, can alter the emotional state of the person, as studies reveal in the presence of fibromyalgia and in other pathological situations.
It is possible to suppose that an emotional allodynia could be established originating from constant myofascial non-physiological afferents, which would bring the emotional state and the myofascial pathology to the same level. In fact, the very position of the body stimulates the areas of emotionality, and the presence of myofascial alterations leads to postural alterations. A dysfunctional myofascial system alters the posture and the emotional state.”
After all, what is FIBROMYALGIA but an extreme state of ADRENAL FATIGUE (some might call it Sympathetic Dominance), many times to the point the body has burned its adrenal glands down to a frazzle (yes, ‘frazzle’ is a scientific term!).
Think about it like this; I personally periodically deal with TRIGGER POINTS. When they get fired up, you had better believe they effect my emotions. And yes, POOR POSTURE affects the whole thing because trunk flexion (a bent-forward or HEAD-FORWARD POSTURE) aggravates the whole mess. And while it’s easy to dismiss this as a purely mechanical / biochemical phenomenon, Bordoni clearly shows that it is neurological and biochemical as well.
Speaking of neurological, Bordoni and Zanier teamed up yet again for a 2013 study called Cranial Nerves XIII and XIV: Nerves in the Shadows. If you’ve ever studied anatomy, the very title of this study will surprise you because there are only 12 Cranial Nerves (always named according to their corresponding Roman numeral — for instance, THE VAGUS NERVE is CN:X or Cranial Nerve Ten). There are no such things as CNXIII or CNXIV —- or are there? I am not going to dwell on this study, but instead will highlight for you a single paragraph having to do with fascia.
“The current view is that nerve N has the ability to affect sexual behavior… . It is believed to act by stimulating luteinizing hormone-releasing hormone on contact with pheromones, improving olfaction and identifying odors, and this series of events will affect sexual behavior.
Finally, the trigeminal system can be stimulated by odors. If a connection between the cervical sympathetic ganglia, the trigeminal system, and the aforementioned nerve [Nerve N] was confirmed, we might better understand and explain some cervical [neck] disorders, such as those related to the menstrual cycle or chronic rhinitis [chronic sinus]. In addition, we could link certain sexual behavioral disorders to trigeminal pain.
In order for the body to maintain homeostasis, each and every part needs to be in harmonious and tensegritive collaboration, with regard to not only fascial but also immunological, neuroendocrine, and psychological functioning.”
Now, we’ll take a look at the way that fascia is both affected by and affects movement, as well as it’s relationship to the nervous system.
FASCIA, MOVEMENT, FIBROBLASTIC ACTIVITY, AND YOUR NERVOUS SYSTEM

As I said at the beginning of today’s post, there are an increasing number of scientists and physicians who strongly believe that the fascia is the key to understanding both health and disease. Much of this has to do with the way that fascia acts on the nervous system. The periphrial nerves in your body are surrounded by three layers of fasica — endoneurium, perineurium, and epineurium (HERE).
When the gliding of these layers on each other is compromised by some sort of adhesion or restriction, Bordoni stated in 2015’s Reflections on Osteopathic Fascia Treatment in the Peripheral Nervous System, that….
“….there is an impediment to the sliding of the nerve, [causing] the rigidity of its fascial structures during joint movement to be increased…. All this will lead to fibrous adhesions, decreasing the sliding of the intrafascicular tissue. The fibrosis increases the compression both inside and outside the tissues with a thickening of the nerve. This is even more noticeable when the nerve passes through small areas. The situation described will generate pain symptoms.”
This is only one of many reasons its critical to keep your fascia moving. Speaking of moving fascia….
In my post on TENSEGRITY, I embedded a clip of Dr JC Guimberteau’s Strolling Under the Skin. In it you can see the way that fascia moves, and the fact that each individual strand of connective tissue moves in ways that are almost impossible to believe, and frankly impossible for me to explain. Last year Bordoni published a study called The Indeterminable Resilience of the Fascial System in which he stated of fascia’s structure….
“These microvacuoles (a repetition of polyhedral units of connective fibrils) under internal or external tension change shape and can manage the movement variations, regulating different body functions and ensuring the maintenance of efficiency of the body systems.
Their plasticity is based on perfect functional chaos: it is not possible to determine the motion vectors of the different fibrils, which differ in behavior and orientation; this strategy confers to the fascial continuum the maximum level of adaptability in response to the changing internal and external conditions of the cell. The fascial continuum is like a flock of birds flying together without a predetermined logic and maintaining their individuality at the same time.”
So, when fascia is working, it’s essentially an elegant “chaos,” but what about when it’s not? On my site I frequently discuss “MICROSCOPIC SCAR TISSUE“. Scar tissue is different than normal tissue in in a variety of manner — it’s less elastic, more pain sensitive, weaker, and less vascular, making it prone to diminished vascularization and oxygenation.
As you might have suspected, the whole mess is prone to both pain and re-injury. Not a good situation. Is there a viable solution? There is, and it has little to do with THE “BIG FIVE”. What it does have to do with is tissue deformation. Bordoni revealed this in 2015’s Understanding Fibroblasts in Order to Comprehend the Osteopathic Treatment of the Fascia.
“The various layers communicate by a microvacuolar system, which is in turn composed of the same structures of the superficial fascia; it is a microscopic web, concerning vessels and nerves, in varying directions, and is highly deformable.”
I mentioned tissue deformation earlier and told you that it is accomplished by putting mechanical stress / loads on the connective tissues like fascia. In many cases, tissue deformation involves varying degrees of “CONTROLLED TRAUMA” to break the adhesion (an “UNTETHERING” if you will) so that said tissue can be progressively loaded (stretched) and untangled, and later on, strengthened.
Dr. B went on to talk about the FIBROBLAST as being the, “foundation of the fascial system.” What makes STIMULATIING FIBROBLASTIC ACTIVITY — stimulating the very cells that make COLLAGEN — so foundational to the healing process? Listen to these cherry-picked reasons.
“The fascial system can be plausibly considered a memory organ, because it not only registers the functions of the structures it surrounds and connects, but also memorizes any function or information arriving and departing from the same structures. The fibroblasts contain receptors for the growth hormone (GH), and depending on the levels of growth hormone circulating they can secrete insulin-like growth factors (IGFs).
The cells of the fibroblasts directly affect contractile tissue repair. They secrete different soluble substances, such as insulin-like growth factors (IGFs), fibroblast growth factors (FGFs), hepatocyte growth factor (HGF), interleukins (ILs), and nitric oxide (NO), as response to mechanical information undergone by the muscles. The cannabinoid receptor or CB1 can be found in the fascial system and in the fibroblasts as well.
This relationship is believed to better manage any inflammation and pain information originating in the fascial tissue, as the fascia undergoes continuous remodeling during the day. Fibroblasts regulate the pressure of fluids and the flow of liquids that permeate the fascia. When the fibroblast undergoes a strain, the water inside is expelled toward the extracellular matrix. Every fibroblast is potentially aware of the functional state of the one close to it, as well as those distant from it, ensuring the fascial and mechanical continuity.
They convey tension, dynamically affect mechanical tension, can rapidly remodel their cytoskeletons, When the fascial tissue lengthens, the fibroblasts flatten themselves and expand, increasing their area of action, are capable of metabolic responses…. This mechanism is known as mechanotransduction; tension is the ‘language’ of cells.”
Holy Toledo that’s amazing! You can start to see why I’ve written OVER 150 ARTICLES ON FASCIA! Believe me when I say that the quote above could have been longer (I cherry-pick everything due to constraints on time and space). One other thing the fibroblasts do is help the fascia align itself so as to direct muscle fibers in the optimal direction / vectors, which creates both power and ease of motion. But what happens when something goes wrong, when the fascia is not “aligned” properly, and motion becomes anything but easy?
Although there are an endless number of ways to therapeutically affect the fascia, the goal is fairly universal. Increase function, while decreasing pain. Bordoni talks about “altering the mechanical properties of fascia, such as density, stiffness, and viscosity, so that the fascia can more readily adapt to physical stresses.”
Some of this you can do yourself (STRETCHING, EXERCISE, FOAM ROLLERS, STEEL ROLLERS, “FUNKY GIZMOS,” TRAMPOLINES, WHOLE BODY VIBRATION THERAPY, all sorts of FUNCTIONAL TRAINING, EXTENSION THERAPY, THE DAKOTA DEVICE, YOGA, PILATES, etc, etc, etc). Some of it you’ll have to have someone do for you / to you (HERE’S ONE). The bottom line is that there must be “breaking of the fascial cross-links” — the fibers that act like extra fibers in a net (HERE is a picture).
When treatment is done properly (note that this is more than a mechanical issue — stick around to the end), “Fibroblasts are able to change their orientation and probably their mechanical behavior.” The end result is an “improved sliding of the various fascial layers, allowing resetting the afferent of the free nerve endings, resulting in physiologic response of the efferent.”
In English this means that when you take abnormal pressure off of the sensory side of the nervous system, it allows the motor side of the system to function better, with the end result being better function and less pain. But what about scar tissue that is stubborn or too deep to access easily?
FASCIA, SCAR TISSUE, AND FAILED SPINAL SURGERY
It was Donnie Iris who famously stated in 1981’s hit single, LOVE IS LIKE A ROCK, that, “you can’t depend on your doctor.” Although some might debate the veracity of his statement, when it comes to effectively dealing with health problems related to fascia, it’s not only true, with the average doctor it’s doubly true. I’ve given you a small taste of how bad scar tissue can be, but we’re going to let Dr. Bordoni (along with Dr. Zanier) give us the bigger picture.
The duo kicked things off in their 2013 study (Skin, Fascias, and Scars: Symptoms and Systemic Connections) by saying, “There are four main stages in skin healing: hemostasis, inflammation, proliferation, and remodeling.” Although I’ve talked about these in the past using slightly different names (HERE), allow me to take just a second to cover them for you again.
- HEMOSTASIS: Hemostasis is when the heme (the blood) becomes stagnant (stasis). This is the formation of the “clot” that contains all of the growth factors, platelet factors, and other anticoagulants, that begin the process of shoring up a “hole” (injury) in the tissue.
- INFLAMMATION: Inflammation (see my earlier link) is neither swelling nor infection. It is a group of chemical messengers that allows the body’s cells to communicate with each other. Just remember that in the correct dose, local inflammation is vital for the healing process. When there is too much however — especially when it is coursing throughout the whole body — it is the chief driver of most disease processes; even those that most people have been led to believe are “genetic”.
- PROLIFERATION: Proliferation is exactly what it sounds like — a proliferation of the collagenous tissue. “Within 8–14 days from the injury, the third healing stage begins, involving the migration of the fibroblasts toward the provisional extracellular matrix made of fibrin and collagen. The fibroblasts, which are stimulated by the different growth factors, are divided into myofibroblasts comparable with smooth muscle cells (they hold a protein, which is the alpha smooth muscle actin). These cells can increase the traction force, and thus they contract and reduce the open area of the lesion.” This is the phase that lasts up to six weeks, which is why insurance companies like to hound those who have been in WHIPLASH ACCIDENTS that the “science” says that treatment beyond a couple months post-accident is not warranted because all the healing that’s going to take place has already taken place.
- REMODELING: Up to this point the scar is a jumbled mess — a wad of fibrous tissue that is functionally similar to a hairball (HERE). “Remodeling” simply takes the scar and makes it more functional — hopefully more like well-combed hair. “Remodeling can last for years and depends on the size and nature of the wound. In this phase, type 3 collagen is replaced by a stronger fiber such as type 1 collagen, but it is lined up without a specific order and is smaller than the collagen of an undamaged skin surface. This results in more strength but less elasticity.”
The question now becomes, what causes scar tissue to go haywire, and what can be done to get the healing process back on track? Let’s talk about what we know — things mentioned in the study. Firstly, inflammation always leads to fibrosis (HERE). So, if at any point in the process, you can control “SYSTEMIC INFLAMMATION,” you’ve helped control the amount of “fibrosis” the body is laying down.
When talking about Sympathetic Dominance and increased inflammatory response (something I mention HERE), the authors mentioned that “We can logically assume that in the presence of a scar, these receptors may experience an alteration, resulting in transmitting nonphysiological signals and creating a pathological reflex arc.” This would account for the Central Sensitization and Complex Regional Pain Syndrome (it used to be called Reflex Sympathetic Dystrophy) mentioned earlier in the post.
Drs. B & Z also discussed people who genetically build great deals of scar tissue (HERE), as well as the direction of the injury and subsequent scar tissue (LANGERS LINES). Not surprisingly both mechanoreceptors and nociceptors are affected by scar tissue, particularly if it’s being exposed to chronic inflammation (HERE).
“We can logically assume that in the presence of a scar, these receptors may experience an alteration, resulting in transmitting nonphysiological signals and creating a pathological reflex arc. It is worth remembering that the language of the cell is, precisely, the tension, which activates the mechanotransduction (ie, the chemicobiological and metabolic response to the tension). This response will be different depending on how the tension emerges and depending on different parameters.
However, it is usually ignored that if the tissue where the tension is observable is in an unbalanced condition, as in the case when a scar is present, the cells cannot properly interpret the message, giving consequent anomalous responses. Fascial tissue is made of contractile fibers, which may possibly produce spasms and consequential dysfunction and pain”
The authors go on to talk even more about the relationship of fascia to the sympathetic nervous system, once more providing a glimpse at potential mechanisms of Sympathetic Dominance and whole body symptoms (make sure to see my suggestions for toning down the sympathetic response — HERE). And this is where things start to get wild.
Bordoni talked about the fact that both sensory and motor nerves carry things other than electrical impulses (“chemicobiological, neurotrophic, and at the same time, immune substances“), potentially causing scar tissue to transmit a wide variety of aberrant messages to the brain and various parts of the body. This is at least part of what creates such a wild array of the bizarre and seemingly unrelated symptoms seen with chronic soft tissue injuries — especially when the HEAD is involved (these people are often labeled by their doctors as “crazy”).
“When there is a fascial injury, there is a fascial dysfunction. A physiological alteration in any part of the body will affect, as a result, everything that is covered by the connective sheet: the symptom will arise in the area concerned with the alteration or, in contrast, in a distal [distant] area, when this is not capable of adapting to the new stressor.”
Bordoni goes on to compare / contrast ankle injuries to spinal injuries, talking about how one can affect the other on numerous levels (mechanical, biochemical, neurological, etc). Pay attention to this direct quote.
“We can then assume that if a scar on the ankle creates an adhesion, this unusual tension will also be recorded by the thoracolumbar fascia, with the consequent appearance of back pain or dysfunctions in the shoulders. It is acknowledged that the thoracolumbar fascia can cause lower back pain or anomalies in the arthrokinematics of the shoulders. Furthermore, when the fascial surface is not in its normal physiological condition, the normal fascial receptors can develop into nociceptors, with a more complex symptomatology.
The sympathetic nervous system is connected to the emotions, and we can assume an emotional alteration resulting from nonphysiological information arising from the periphery. We can still hypothesize the presence of thalamic and hypothalamic dysfunctions because of relations with the sympathetic system and skin. We can also logically theorize that in time, a scar on the ankle might generate a visceral dysfunction.”
Allow me to summarize. A high-flying basketball player roaches his ankles several times, causing fascial and TENDINOUS dysfunctions. Coupled with systemic inflammation from living the HIGH CARB LIFESTYLE (it’s what “healthy” people were doing in the 1980’s), he develops problems in the THRORACOLUMBAR FASCIA that creates a degree of chronic low back pain as well as LEVATOR TRIGGER POINTS behind the shoulders.
The mechanoreceptors found in fascia are actually converted to nociceptors (pain sensors), that ratchet up the sympathetic side of the ANS (autonomic nervous system). This can actually lead not only to chronic pain but to problems in the viscera (the organs). It also, as I showed you earlier, changes ones emotions. How do I know this? After three separate avulsion fractures of my ankles (right twice, left once), I was at one time ready to have my right ankle amputated until THIS HAPPENED.
Through changing my diet, methods of exercise, and improving the ways I treat myself, I am about 90% better than I was 12 or 14 years ago. Although I never want to go back there again, the experience undoubtedly led to a better understanding and dogged determinedness to help those suffering with their unique problem(s).
As for surgeries, Bordoni and Zanier went on to talk about SPINAL SURGERY, ABDOMINAL SURGERY, KNEE SURGERY, and several others. They also talked extensively about the potential problems associated with said surgeries — adhesions, scar tissue, chronic pain, pathological biomechanics, muscle spasms, visceral dysfunction, ABNORMAL PROPRIOCEPTION, along with dozens of others.
It’s why I always suggest conservative methods before trying surgery. Listen to what they say about the potential far-reaching effects of a surgery on the low back, including its ability to adversely affect the Cervical Fascia and / or cause TOS.
“A lumbar scar could increase the tension of the deep fascia of the neck, pulling the stellate ganglion. This event may cause symptoms at the level of the cervical and thoracic outlet and negatively affect all the neural structures related to it. To exclusively treat the joint negatively involved will not solve the problem.”
What does solve the problem? Although there are many thought processes, Bordoni and Zanier discuss solutions in another 2015 study called A Multidisciplinary Approach to Scars: A Narrative Review. Here are some of the methods they mention in their study.
Clear the HPA-AXIS, control inflammation, make sure your body is dealing with OXIDATION, HYPERBARIC O2, OT, PT, DO, CHIRO, MASSAGE, BODY WORK, NEEDLING, CUPPING, HERBAL, Ayurvedic, homeopathic, or naturopathic remedies, NUTRITIONAL SUPPORT, along with several others. But what happens when these approaches fail and you are forced to have surgery?
In 2016, Bordoni came back with a study called Failed Back Surgery Syndrome: Review and New Hypotheses. What’s interesting to me is how he shows studies on back surgery are literally all over the place. “The percentage of pain detected after spinal surgery varies ranging from a low of 5% to a high of 74.6%, and the percentage of need for re-operation ranging from 13.4% to 35%.” This is yet another example of NOT BEING ABLE TO TRUST STATISTICS.
Because we’ve covered most of the basics of why a back surgery might fail, I am going to mention the one that most people are totally unfamiliar with, the diaphragm. “One component that is not even considered when trying to understand the reasons for failed back surgery syndrome is dysfunction of the diaphragm muscle, which is not referred to in the literature. The diaphragm is involved in chronic lower back and sacroiliac pain and plays an important role in the management of pain perception.” Which brings us to our next section……
BREATHING AND FASCIA’S RELATIONSHIP TO THE DIAPHRAGM
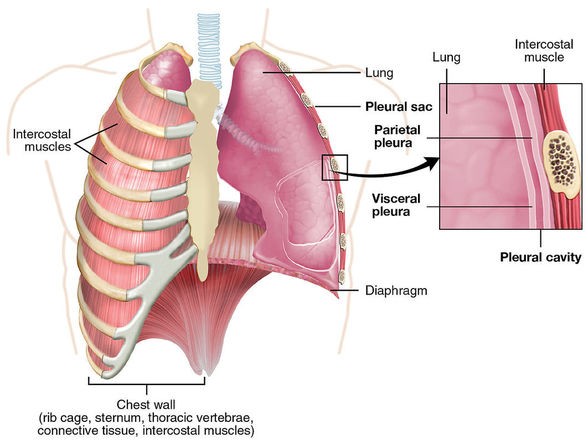
If you click on the pics above, you can blow them up and take a look at the relationship between the muscle we call the diaphragm, the abdominal cavity, THE RIBS, and the spine. Although Bordoni is one of the world’s foremost experts on fascia, his niche would have to be the diaphragm. In 2013, Bordoni and Zanier published a study on this topic called Anatomic Connections of the Diaphragm: Influence of Respiration on the Body System.
“From a functional perspective, two areas can be recognized in the diaphragm, ie, the crural region and the costal region. The former is responsible for correct breathing, whereas the latter prevents gastroesophageal reflux. This separation has an anatomic function, because during deglutition [swallowing], esophageal distention, and vomiting, these diaphragmatic areas must work at different times and with different innervations [nerves].”
This brief video shows the bony attachment points of the diaphragm. Notice how when it contracts it pulls downward, causing negative pressure in the thoracic cavity to “draw” air in, while when it relaxes, it pushes air upward and out.
Listen to what the authors say about the pelvic diaphragm (pelvic floor) in relation to breathing. “The pelvic diaphragm not only has a significant role in supporting the pelvic organs and in resisting increasing pressure, but also affects respiratory function.” And while I will not cover it here, the authors dealt at length with the diaphrgm’s numerous neurological connections (including the phrenic nerve), saying “It is important to emphasize that when an organ such as the liver or the gallbladder does not function properly, the phrenic nerve will be affected.”
Yet another example of everything affecting everything (and be honest; how crazy common are LIVER / GALL BLADDER issues in the Westernized world?). Speaking of EVERYTHING BEING CONNECTED (“the deep cervical fascia reaches the pubis via the fascia transversalis“), let’s take a look at the study’s section called Fascial Connections.
“It is important to consider the fascial and connective links between the diaphragm and the pelvic floor, and the rest of the body. First, the abdominal muscles are related to the costal, lumbar, and pubic iliac regions of the body, ie, rectus abdominis, the internal and external oblique muscles, pyramidalis, cremaster, transversus abdominis, great psoas, quadratus lumborum, sacrospinalis, and transversus spinalis (where the multifidus spinae is distinguishable).
Further, the fascial tissue possesses fibers capable of contracting, probably causing spasms, followed by dysfunction and pain. When there is a problem in the diaphragm or in any of the structures belonging to this fascia, there will be dysfunction. A physiologic alteration in any part of the body will affect everything that is covered by this connective sheet: the symptom will arise in the area concerned with the alteration or in a distal area, when this is not capable of adapting to the new stressor.
If handling of these forces is restrained, postural and visceral equilibrium will become dysfunctional. We can assume that the phrenic nerve passes through the deep fascia and media, and be indirectly affected by the superficial fascia of the neck.”
Interestingly enough, Bordini not only talked about reflux and PPI drugs in this study, just last month he published a study called Low Back Pain and Gastroesophageal Reflux in Patients with COPD: The Disease in the Breath. I’ve talked to you about GERD and the dangers of PPI’s (Proton Pump Inhibitors — aka “acid blockers”), as well as giving you a posts on both CHRONIC LOW BACK PAIN and COPD.
Bordoni and his team put the whole thing together, showing you not only how common all of them are in our society, but just how intimately related to each other they are as well. Although I have dealt with it on my site, the question now becomes, how do you successfully address the issue without drugs?
In 2016, Bordoni published a study on this very topic called A Review of Analgesic and Emotive Breathing: A Multidisciplinary Approach, in which his team stated…
“The diaphragm is the primary muscle involved in breathing and other non-primarily respiratory functions such as the maintenance of correct posture and lumbar and sacroiliac movement. It intervenes to facilitate cleaning of the upper airways through coughing, facilitates the evacuation of the intestines, and promotes the redistribution of the body’s blood. The diaphragm also has the ability to affect the perception of pain and the emotional state of the patient.”
After going on to talk about the many neurological and mechanical connections between breathing, the diaphragm, and the problems mentioned above, he suggests the solution.
“It is undeniable that a respiratory disorder can alter the emotional picture, similar to depression and anxiety, and it is equally true that an altered emotional state worsens the respiratory function. Considering also the emotional side during manual treatment, such as manual therapy or an osteopathic treatment, would probably be more helpful for the patient.”
I would add to that, learning how to breathe properly. While I will not go into this topic in depth, realize that there are different schools of thought on exactly what “proper breathing” should look like. A number of years ago I met a gentleman from Switzerland (actually this guy was in his 60’s and looked and sounded like a smaller version of Arnold in his prime), who had cured (his word, not mine) a number of major health problems using the Buteyko Method of breathing, developed by a Russian MD, Konstantin Pavlovich Buteyko, back in the 1950’s.
He gave me a couple of E-books on the subject, which are fascinating to say the least, the premise being that controlling your CO2 levels is far more important for all aspects of breathing and health that O2 levels.
There is one more study I need to mention before heading to the final section — last year’s The Five Diaphragms in Patients Following Cardiac Surgery in Sternotomy: An Observational Study. The authors, led by Dr. B, looked at and examined 300 patients that had been cut from stem to stern during open-heart surgery.
The study had a great deal to say about the fascial system as related to the body’s five different diaphragms —- the respiratory diaphragm, pelvic floor, buccal diaphragm (the cheek), the thoracic outlet (where TOS occurs), and the tentorial diaphragm (made up of the tentorim cerebelli or membrane that separates the brain / cerebrum from the cerebellum).
“The fascial continuum creates a structural continuity that gives form and function to every tissue and organ. The human body must be considered as a functional unit, where every area is in communication with another through the fascial continuum, consequently originating perfect tensegritive equilibrium.
The dural fascia system of the skull continues, coming into contact with the deep cervical fascia, continuing with the endothoracic fascia anteriorly and the thoracolumbar fascia posteriorly; the first continues with the transversalis fascia until the pubis, while the second involves the whole of the posterior area of the body. This fascia system involves all the bodily diaphragms, including the respiratory diaphragm.
Trauma following a cardiac surgery with a sternotomy will affect all the diaphragms as a result of the anatomic and neurological continuity. The evaluation has highlighted the structure of fascia restrictions and the preferential positioning of such structures. The diaphragms of the body are considered a pivotal point in the interpretation of the patient’s clinical status and treatment.”
FASCIA, DEPRESSION, ANXIETY, HEART FAILURE, AND MANIPULATION

Just last month Bordini published a study in Future Cardiology called Depression and Anxiety in Patients with Chronic Heart Failure. I’ve shown you in the past how DEPRESSION is linked to any number of health-related problems (including heart problems), via INFLAMMATION. This latest study strengthens this link. His study, of course, has a strong emphasis on the diaphragm, but goes beyond that.
After talking about the sheer numbers of people as well as the astronomical costs associated with caring for said people, Bordini got down to the brass tacks of the study. In a phrase that could have easily gone in the section above….
“The inspiratory dysfunction of the diaphragm is a key element in patients with chronic heart failure, influencing mortality and morbidity rates. The breath becomes more superficial, with increase of the sympathetic activity; the sympathetic nervous system stimulates the phrenic afferents, which in turn stimulate the sympathetic fibers, in a vicious circle. This pathological condition predisposes the patient to arrhythmias and higher risk of sudden death.”
The authors went on to discuss the VAGUS NERVE (use it to your advantage to counteract Sympathetic Dominance), and the way it can become compromised……
Emotional conditions such as anxiety and depression can negatively affect the baroreceptors’ response [pressure receptors in blood vessels used to adjust B], as well as they can produce an altered function on the diaphragm. The action of the diaphragm is not only controlled by metabolic factors, but also by emotional states such as sadness, fear, anxiety and anger. The interaction between the breath and the emotions involves a complex interaction between the brainstem and a few brain centers…
The breath stimulates the mechanoreceptors of the diaphragm and the visceroceptors of the viscera [organs] moving during the respiration, which constitute the interoception mechanism. A dysregulation in the interoceptive pathways could cause a distortion of the body image, affecting the emotional condition. Anxiety can alter a few afferent pathways related to breathing, amplifying one or more receptor pathways related to the respiration. The phrenic and vagus nerves provide visceral information.
The authors went on to talk about the way that abnormal stretching of peripheral nerves affect the ability of the fascial sheaths of said nerves to slide on each other properly. This is a big deal because the sliding of the fascial layers is a huge source of PROPRIOCEPTION / MECHANORECEPTION, which, as you already know if you’ve seen the post that has over 50K likes on Facebook, is responsible for everything that occurs in the body (and one of the reasons that growing numbers of scientists and physicians feel that fascia holds the key to solving most disease processes).
In fact, these authors discussed the ways that functional problems in this system cause (I am loosely quoting here) ‘pain, anxiety, depression, intense emotions, neurogenic neuroinflammation, trouble breathing, functional impairment of the muscle tissue, further destabilizing the function of the diaphragm, as well as problems in the hormonal system and brain itself (the hypothalamus–pituitary axis),’ affect the rest of the body. Even for you Yoga Masters out there, who knew that breathing was this big a deal? BTW, the next logical question is how to successfully affect the fascia to improve cardiovascular function and breathing?
Although I’ve already touched on this, in a study from October of 2015, Bordoni answered this question via a study titled The Fascial System and Exercise Intolerance in Patients with Chronic Heart Failure…. After talking about the relationship between inflammation, Sympathetic Dominance, OXIDATIVE STRESS, and heart failure, Dr. Bordoni went on to say…
“The literature, however, recognizes fascial dysfunction as a cause in many pathological situations. The fascial system, if altered, generates a symptomatology that deteriorates the health condition of the patient, who very often develops symptoms that are more significant than the clinical parameters diagnosed through medical diagnostic devices.”
These are the same tests and parameters that frequently tell doctors that there is nothing wrong with you.
“Chronic fatigue, for instance, can be associated with the fascial system, particularly when the pathological disorder has persisted for several years. A recent experimental study has shown that common physiological mechanisms may be involved in the causation of muscle pain and fatigue; the nociceptive afferent [pain] inputs from the fascial system can modulate the afferent response from the central nervous system. If the afferent is not physiological, the efferent [motor side of the nervous system] will be in dysfunction and pathology.”
Affect the motor portion of the nerve and you affect everything. That would be everything with a capital “E”. “Muscle fatigue is associated with a decline in motor coordination and performance. The fascial continuum is essential for transmitting the muscle force and for correct motor coordination: the fascia is a vital instrument that enables the individual to communicate and live independently. The transmission of the force is ensured by the fascial integrity, which is expressed by the motor activity produced.”
In other words, FASCIAL ADHESIONS are going to adversely affect the way your body’s various parts communicate with and respond to each other, in turn affecting your bodies ability to function as normal on almost any plane you care to discuss. This is why dealing with said adhesions is a big deal. Here is a loosely quoted list of the benefits of manual therapies.
“Improve motor coordination, reduce metabolic expenditure, decreased intolerance to exercise, increase proprioception, reduce inflammation and influence anti-inflammatory cytokines, affect the intramuscular pH, modulate acid/base parameters, modulate the temperature of the extracellular matrix, better removal of waste metabolites, favor production of hyaluronic acid, increase fibroblast growth factors (FGFs), hepatocyte growth factor (HGF), ILs, and nitric oxide (NO), improve coordination and posture, improve tone, improve biotensegrity, improve urinary incontinence, and positively affect breathing.
Working on these interconnected parts of the body in terms of fascial and neurological links; it is possible hypothetically to create an improvement in the patient’s symptoms, due to the improvements of the fascial system. Evidence-based medicine is based not only on scientific research highlighted in articles, but also on the patient’s experience of treatment and the clinical experience of the operator.”
The end-product, according to a study published last July in the Annals of Thoracic Surgery is that Osteopathic Manipulative Treatment Improves Heart Surgery Outcomes. In this RCT, eighty post-op heart surgery patients were divided into two groups — the first getting post-surgical respiratory therapy alone, and the second getting manual therapy along with. What were the results? Only that group two had shorter hospital stays, lower pain scores, and better breathing as measured by spirometry.
When you look at the big picture, Bordoni’s work proves not only see how big a deal fascia is, but that it’s important to deal with injury or dysfunction ASAP. That’s because in most cases, adhesed, thickened, or densified fascia can be changed (“deformed“). The thing to remember here is that your approach must be multi-faceted. In other words, don’t even think of tackling serious problems solely in a mechanical fashion.
Address adhesed fascia on all levels (including controlling inflammation) and it’s more likely to get results LIKE THESE. But fail to change crappy diets or unhealthy lifestyles means you will probably be working against yourself as you continue to drive fibrosis-causing inflammation. And as for those things you can do to help your own cause fascia-wise, they are legion and for the most part contained in MY GENERIC POST on “Universal Cures” (the word ‘cure’ being used figuratively of course). And the best thing about it for you is that it’s completely and 100% free!
