The first thing I want you to understand when reading this post is that when I talk about “torn fascia” in this context, I am not talking about a COMPLETE RUPTURE OR HERNIATION of the fascia — the sort of thing that leaves a visible bulge. I am talking about a disruption of the normal organized structure of fascia on a cellular level — sort of like a HAIRBALL -vs- WELL-COMBED HAIR microscopically speaking. I’ve previously shown you how fascial adhesions occur (HERE), and I’ve shown you in several posts why fibrotic tissue / scar tissue is bad news on multiple levels (HERE and HERE). Today I want to talk a bit about what they can look like clinically, and to do that I am going to give you an example that occurred in my office earlier this week.
A young lady came see me yesterday, who had been struggling with low back pain for over two months. She is of normal weight, active, and appeared to be quite fit. In the course of my examination, I realized almost immediately that even though she had none of the other signs that might indicate a disc issue (HERE are the red flags for disc) and no history of trauma; when I asked her to touch her toes, she could not bend forward more than just a few inches. Other than having diffuse pain fairly close to her spine (more left sided than right) the rest of her low back exam was fairly unremarkable (she did, however, have some serious restriction in her neck that I will talk about later). The next thing I did was check her Thoracolumbar Fascia and surrounding tissues for FIBROSIS.
After working on her a bit, I noticed a couple of things. Firstly, because I often treat / test / treat / test / treat / test many times during a visit, it didn’t take more than a few minutes to see dramatic improvement in her ability to bend forward. Although I could not get her to the point where she could touch her toes on this visit, she managed to get within about 12 or 14 inches — a massive improvement over being almost totally unable to forward bend. The thing I really want to share with you, however, is the tear.
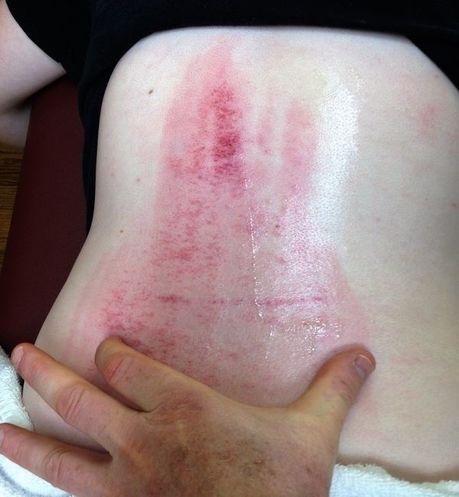
While it’s not uncommon to see this sort of thing in the form of a visible “STRETCH MARK,” this was not the case here. Her tear could be seen as a line about five inches long, stretching over her spine, across both sides of her back, and completely invisible until I started working on her. And although not the case with this patient, sometimes when I find a tear like this, I find lots of FASCIAL ADHESION either above or below the tear, with virtually nothing opposite. What does any of this really mean? While I’m not totally sure, suffice it to say that Scar Tissue is restrictive, and restricted tissues are never a good thing.
I would have to say that this case is yet another proof that the study I wrote about YESTERDAY is spot on — that Thoracolumbar Fascia is a common generator of low back pain. Furthermore, I firmly believe that in similar fashion to the drugs commonly given for problems like hers’ (THE BIG FIVE), lots and lots of chiropractic adjustments (HERE), lots and lots of therapy (HERE), or lots of any number of other treatments, can really only hope to cover the symptoms. If a problem like this is not treated like a CARNIVAL GAME (yes, you had better click the link), then long-term relief, and more importantly, an actual resolution of said problem, will not be achieved, eventually leading to degenerative changes via proprioceptive loss (HERE).
Sure, she needs to do some CORE STRENGTHENING EXERCISES and address any UPPER CROSSED and LOWER CROSSED SYNDROME that is present (we’ll get to that, and frankly, she can do it on her own). But without some kind of bodywork to deal with the underlying “TETHERING EFFECT” of the torn and subsequently scarred fascia, solving this thing will prove elusive.
For the record, because of certain characteristics of this young lady that I am not going to talk about right now, I have a suspicion that she is GLUTEN INTOLERANT. What makes me wonder? She is having HEADACHES every day, and has a great deal of restriction in her neck in all ranges, despite no history of traumatic injury there either. Any time I see problems both above and below the waist, as well as on both the right and left sides of the body, it raises red flags as far as underlying inflammation is concerned. Dietary changes just happen to be the lowest of the low-hanging fruit — the easiest thing for her to address on her own, and one of the quickest to potentially see results with. I have already suggested that at some point in time, she do an ELIMINATION DIET to figure out for sure.
