ESSENTIAL FATTY ACID METABOLISM AND INFLAMMATION: ANOTHER REASON THAT PALEO IS SUPERIOR TO LOW CARB
You’ve only heard me say it about a million times — when it comes to your health, inflammation is everything. The problem is that it’s rare to find people who truly understand what inflammation is, let alone the fact that it’s a necessary component of your immune system (HERE) that can be driven to excess by any number of things, including diet.
Although there are a myriad of things that can cause inflammation, I’ve shown you how certain foods such as GRAINS, DAIRY, FODMAPS, GLUTEN, NIGHTSHADES, etc, etc, etc, have the potential to be inflammatory — for some people, extremely inflammatory. Conversely, there are foods that are anti-inflammatory (ANTI-INFLAMMATORY DIET). Today we are going to talk about how the fats that you consume are either driving or squelching inflammation in your body — fatty acid metabolism and inflammation, or non-inflammation (anti-inflammation) as the case may be.
The first thing you have to be aware of when it comes to fatty acid metabolism and inflammation, it is that it’s not only possible, it’s rather common to see people who have trouble digesting fats. This is frequently due to a lack of DIGESTIVE ENZYMES and diminished function of the liver / gallbladder, although it can certainly come from the pancreas as well (for the digestion of fats, STOMACH ACID is not the critical factor it is for protein). Let’s take a brief look at how the metabolism of fats relates to the amount of inflammation you will deal with on a day to day basis.
DIAGRAM: FATTY ACID METABOLISM AND INFLAMMATION
If you are interested in seeing why the fats that you consume have a huge bearing on whether you are inflamed or not (they are either inflammatory or anti-inflammatory), please take 20 seconds to understand this diagram on fatty acid metabolism and inflammation.
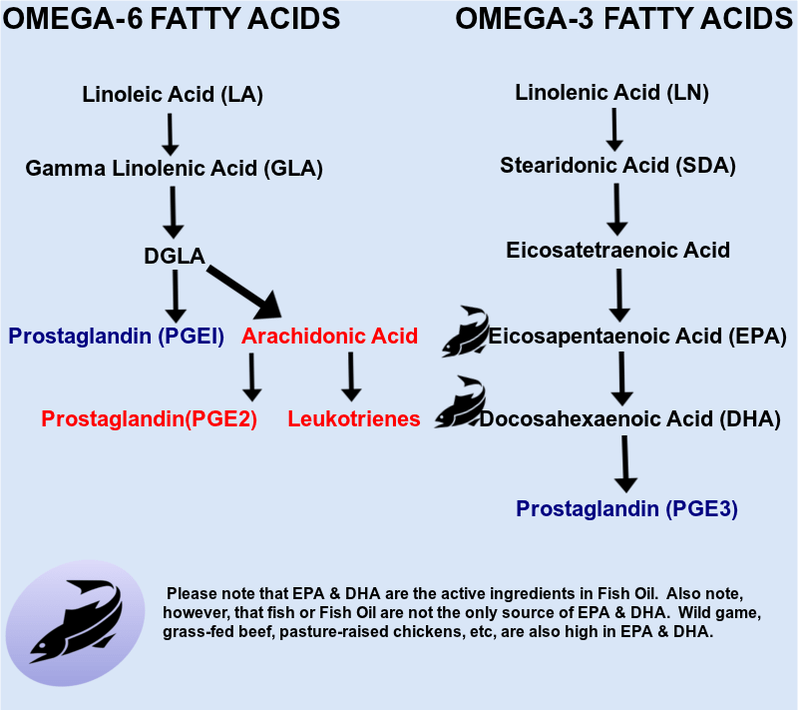
OMEGA-6 FATTY ACID METABOLISM
Although it’s probably an unrealistic goal for most of us, the ideal ratio of dietary Omega-6’s to Omega-3’s would be 1:1 (experts say it should not exceed 3:1). The problem is that when you start looking at studies on fish oil, you quickly see how bad things are in this department (the department of fatty acid metabolism and inflammation).
Thanks to the SAD (Standard American Diet), the ratio is between 25:1 and 40:1. Although Omega-6 fatty acids get a bad rap for being “inflammatory,” this is not automatically so since there are two separate metabolic pathways on this side of the equation; only one of them being inflammatory, the other being anti-inflammatory.
The first fatty acid in this pathway is Linoleic Acid — an essential fatty acid, meaning your body does not make it; it must be consumed dietarily. Unfortunately, most people get way to much LA in their diet in the form of various cheap cooking oils such as SOYBEAN, corn, safflower, and cottonseed oil — oils that are almost universal to heavily processed foods. There is, however, a better form of LA — CLA or Conjugated Linoleic Acid.
Where does CLA come from? It comes from consuming the sorts of fats that were considered deadly while I was growing up — RED MEAT, EGGS, BUTTER, and full-fat dairy (whole milk). It’s important to realize that CLA has numerous health benefits as seen in peer-review, some of which include weight loss (in particular, it helps mobilize and burn fat), hunger control, blood sugar regulation, and down-regulating the part of the immune system responsible for inflammation.
A dysfunction or deficiency of the enzyme that converts LA to GLA (Gamma Linolenic Acid) is yet another way that people skew their Omega-6 metabolism toward the pro-inflammatory AA (Arachidonic Acid) pathway. What are the most common causes of this sort of metabolic dysfunction?
Honestly, it’s the usual suspects — the same actors we see with any number of other health issues — OBESITY, BLOOD SUGAR DYSREGULATION, hormonal issues (including THYROID), ADRENAL FATIGUE (stress as measured by HRV), alcohol and drugs (this includes PRESCRIPTION DRUGS), TRANS FATS, along with any number of others.
The result is a myriad of inflammatory diseases that I have linked to throughout this post. As far as supplementing, the two best sources of GLA are Black Currant and Borage Oils. And while many people use it, the problem you get into with Evening Primrose Oil is that like soy, it tends to be a xenohormone (estrogenic).
DGLA is where we see the Omega-6 pathway split. Depending on any number of factors, most having to do with diet and lifestyle (EPIGENETIC FACTORS), this pathway will either be driven to the left — the anti-inflammatory PGE1 pathway, or the right — the pro-inflammatory pathway that leads to AA (Arachidonic Acid).
While AA is certainly not a bad thing (it is a chief component of CELL MEMBRANES, THE BRAIN, MUSCLES, and liver), too much of a good thing is often a bad thing — exactly what we see with virtually all INFLAMMATORY MEDIATORS. Too many highly processed, frequently rancid, grain, vegetable, and peanut oils, and you are going to make lots of leukotrienes and PGE2 — both of which are highly inflammatory.
Not only that, but LIVING THE HIGH CARB LIFESTYLE is one of the biggest blockers of the PGE1 pathway. As some of you might know, the AA pathway is blocked by NSAIDS and CORTICOSTEROIDS, but the side effects are numerous, accumulative, and potentially brutal.
Despite all the information on this topic, Americans continue to drive the inflammatory side of Omega-6 fatty acid metabolism to excess, thus the title of today’s post — Fatty Acid Metabolism and Inflammation. Since the early 1980’s, hundreds upon hundreds of studies have shown how inflammatory leukotrienes and PGE2 are (they are two of the many cellular messengers we refer to collectively as “inflammation”).
What does peer-review have to say about these two mediators? As much as I would love to take the time to give you a long list of the problems associated with, you can freak yourself out by doing your own research (PubMed). Within five minutes you will realize that both of them (particularly PGE2) are associated with a slew of INFLAMMATORY DISEASES, including nasty creatures like CANCER, ARTHRITIS, DIABETES, and HEART DISEASE.
The anti-inflammatory PGE1 pathway is mostly about promoting circulation and blood flow as seen by numerous studies on PubMed.
OMEGA-3 FATTY ACID METABOLISM
“α-Linolenic acid is relatively more susceptible to oxidation and will become rancid more quickly than many other oils. Oxidative instability of α-linolenic acid is one reason why producers choose to partially hydrogenate oils containing α-linolenic acid, such as soybean oil. Soybeans are the largest source of edible oils in the U.S., and 40% of soy oil production is partially hydrogenated.” From Wikipedia’s entry on ALA
As I stated earlier, Americans over-consume Omega-6’s, while under-consuming Omega-3’s by a factor of 25 to 40, depending on whose research you believe to be most accurate. Furthermore, not all Omega-3’s are created equally. Linolenic Acid (in the form of Alpha Linolenic Acid or ALA) comes from seeds of Chia, Hemp, Flaxseed, Rapeseed (Canola), Soy, and a number of others.
Unfortunately, many ALA supplements use soy because it is cheap and abundant (it also happens to be a PHYTOESTROGEN / XENOHORMONE). I also saw where Perilla (a form of mint that I’ve called “Strawberry Mint” for years — around here it’s considered a weed — is considered a good source, although I’ve heard it’s mildly toxic to cattle). Here’s the rub.
I’ve run into lots of people over the years, who for various reasons, don’t want to take fish oil (even the PHARMACEUTICAL GRADE FISH OIL that has had all the protein removed making it non-burpy). Instead, they think they can get their Omega-3’s by taking flax seed oil. While I am personally a big fan of cold-pressed flax oil, it is critical to understand why it’s not a substitute for animal-based sources of Omega-3’s. It all has to do with the crappy conversion of LN to EPA / DHA. Again, according to numerous studies, and depending whose research you believe is most viable….
- To convert flax seed oil to equivalent amounts of EPA, you would have to consume approximately 15 times the amount of flax oil as fish oil since the conversion is only about 5 to 10%.
- To convert flax seed oil to equivalent amounts of DHA, you would have to consume between twenty to fifty times the amount of flax oil as fish oil since the conversion is even worse — only about 2 to 5%.
The end-product of consuming EPA (it’s better for inflammation) and DHA (it’s better for brain function) is that you produce lots of Prostaglandin E3 (PGE3), which is extremely anti-inflammatory. I could easily sit here and give you study after study on the benefits of PGE3 for a wide array of inflammatory problems. Today I’m only giving you one.
Three years ago next month, the journal Cancer Letters published a study called Prostaglandin E3 Metabolism and Cancer. The authors, three oncologists from the University of Texas and MD Anderson Cancer Treatment Center in Houston, had this to say about EPA and DHA.
“The anticancer activity of Omega-3 fatty acids, especially those derived from fish, such as eicosapentaenoic acid (EPA) and docosahexaenoic acid) (DHA), has been studied for centuries. A number of studies have suggested that the anticancer activities of EPA and DHA are associated with their effects on eicosanoid metabolism by which they inhibit prostaglandin E2 (PGE2) production.”
Here’s what’s amazing about this study. Not only do EPA and DHA promote anti-inflammatory PGE3, they inhibit pro-inflammatory PGE2. This is true whether you are fighting cancer or arthritis, ASTHMA or ADHD, IBS or IBD.
SOME CONCLUSIONS ABOUT FATTY ACID METABOLISM
The first thing you need to understand is that where you get your fats from matters. Dr David Seamans, a FUNCTIONAL NEUROLOGIST and nutritional expert, has a simple rule of thumb when it comes to diet — eat vegetation (not GRAINS) and animals that ate vegetation (HERE).
In other words, the diet of the animal whose meat or by-products (eggs, milk, etc) you are consuming matters because it changes the fatty acid profile. In the scientific literature, FEEDLOT-RAISED MEAT is referred to as “obese” (which is exactly the goal of commercial feeding). Naturally, grain changes the fatty acid profile, skewing it toward Omega-6 and Arachidonic Acid, increasing both inflammation and the likelihood of major weight gain (yes, obesity is considered a disease of inflammation).
The second part of this equation is that there are any number of things that can adversely affect fatty acid metabolism, many of which have been mentioned today in passing. Furthermore, if you take a look at the Fatty Acid Metabolism and Inflammation Chart above, it’s critical to realize that even though I have not included them, there are enzymes driving each and every conversion step.
As I stated earlier, poor lifestyle choices are going to foul these conversions — especially the conversions to PGE1 and PGE3 — the anti-inflammatory part of this equation, while making the conversion to inflammatory AA the default pathway.
As per the title of today’s post, this means that while LOW CARB DIETS (KETOGENIC included) can knock it out of the park as far as controlling the single most important factor as far as your health is concerned (blood sugar), it will not necessarily help you solve your SYSTEMIC INFLAMMATION as greatly as you were hoping it would.
The beauty of the PALEO DIET is that you are eating meats and fats that have been raised in a “SUSTAINABLE” fashion, not only getting the blood sugar benefits of Low Carb, but the fatty acid / inflammation benefits as well as the benefits of cutting the endocrine disruptors / xenohormones / artificial estrogens (see earlier link). It’s largely why I suggest that if you are doing low carb, it’s just a hop, skip, and a jump over to paleo (HERE).
If you are struggling with chronic health issues and are not sure where to turn, realize that your case might require the intervention of a specialist in FUNCTIONAL MEDICINE. Also realize that before going the FM route, there are any number of things you can do to take matters into your own hands and start taking your life back. A basic outline of those steps can be found HERE. No, it’s not a solution for everyone. But following steps that have been proven over and over again in the peer-reviewed scientific literature only makes sense.
