Top-Ten Solutions for Chronic Low Back Pain
Right now in America, there are tens of millions of people struggling with Low Back Pain (LBP). Proof? Allow me hit you with the mind-blowing statistics. For instance, the American Academy of Pain Medicine says that one hundred million citizens live with Chronic Pain. Numerous studies show that at least half these cases are “severe“. Furthermore, several physicians writing for MedScape stated…
“An estimated 15-20% develop protracted pain, and approximately 2-8% have chronic pain. Of those individuals who remain disabled for more than 6 months, fewer than half return to work, and after 2 years of LBP disability, a return to work is even more unlikely. Studies suggest that one third to one fourth of patients in a primary care setting may still have problems after 1 year and is the most common cause of disability in Americans younger than 45 years.
LBP has been cited as the second most frequent reason to visit a physician for a chronic condition, the fifth most common cause for hospitalization, and the third most frequent reason for a surgical procedure. The socioeconomic impact of chronic LBP is massive.”
A 2012 study by four MD / Ph.D researchers and published in the journal Helio (Low Back Pain and Sciatica Prevalence and Intensity…) concluded that, “39.5% of patients reported low back pain 24.6% reported sciatica during the previous 6-month period.”
Bone & Joint Burden dot org said of LBP, “In any given year, between 12% and 14.0% of the United States’ adult population (above 18 years of age) will visit their physician with complaints of back pain. In addition, an unknown, but very high number will visit a chiropractor or physical therapist for these complaints. The number of physician visits has increased steadily over the years. In 2012, more than 52.3 million patients visited a physician with a complaint of back pain.”
A 104 page piece by the drug company Pfizer (The Burden of Pain Among Adults in the United States) revealed that, “29–39% of adults with joint pain, low back pain, and neck pain report arthritis attributable activity limitations.“
The website of the American Physical Therapy Association (Most Americans Live with Low Back Pain – and Don’t Seek Treatment) stated….
“More than one-third of adults say low back pain has affected their ability to engage in tasks of daily living (39 percent), exercise (38 percent), and sleep (37 percent). Low back pain isn’t just for those who spend a lot of time on their feet. In fact, more than half (54 percent) of Americans who experience low back pain spend the majority of their workday sitting.
Men (31 percent) are more likely than women (20 percent) to report that low back pain affects their ability to do work. When experiencing low back pain, nearly three in four (72 percent) Americans use pain medication as a way to relieve their symptoms.”
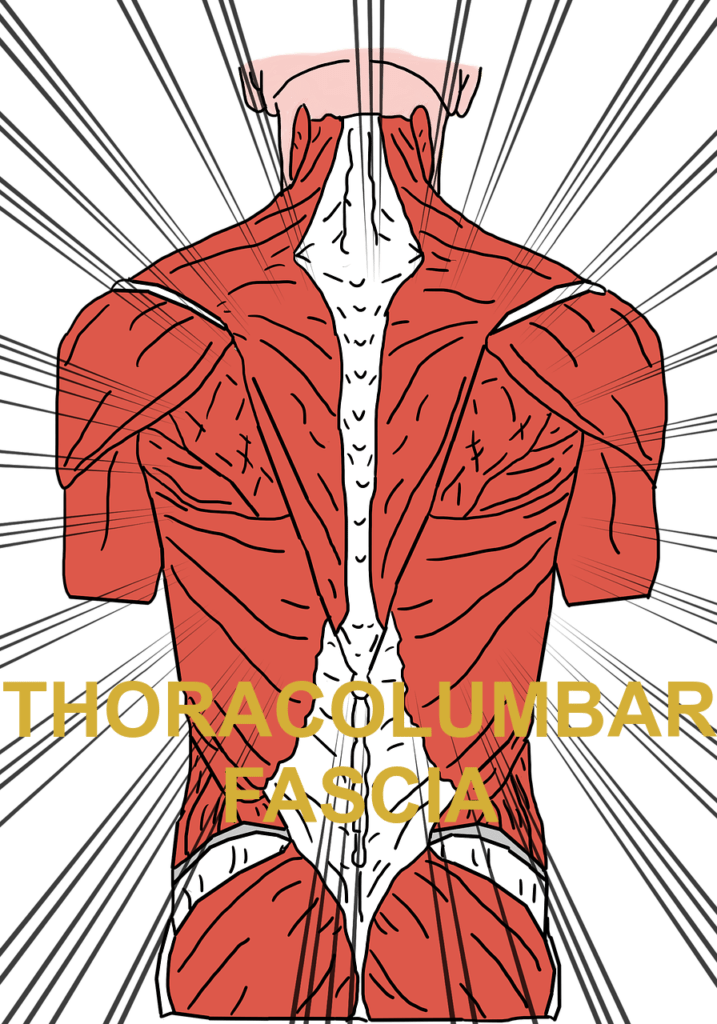
After all of this, the harsh reality is that I am barely even beginning to scratch the surface of this problem of low back pain. But instead of just talking about how bad the situation is, let me give you some insight that might start you down the path to solving your pain by addressing the underlying reasons for the pain. First and foremost, to solve your own back issues it is critical that you have a basic understanding of the Thoracolumbar Fascia.
MYOFASCIAL SLINGS
The Thoracolumbar area is extremely important as far as BIOMECHANICS and your ability to move are concerned. This is because of its unique ability to act as a ‘transfer case’ or ‘axle differential,’ which gives it the unique ability to shift loads and forces from the lower extremities to the upper extremities.
As you might imagine, proper function in this area is critical if you want to successfully heal the tissue damage caused by SPORTS INJURIES, work-related injuries, REPETITIVE INJURIES, injuries due to WHIPLASH, or if you are simply wanting to improve your golf game. This is also why lower body strength is so critical for upper body strength, and should never be neglected — particularly if you are an athlete.
Think of the Thoracolumbar Fascia as the centerpiece of an anatomical “corset”. This corset is actually made up of several corsets that are usually referred to as slings. Some of the various names of these slings include the Posterior Longitudinal Sling, the Anterior Oblique Sling, and the Posterior Oblique Sling. These ‘slings’ relate to something called “Force Closure“.
Force Closure pertains to the muscle’s ability to compress two joint surfaces together via their LIGAMENTOUS, TENDINOUS, and FASCIAL attachments. Although muscular balance must be maintained, an oversimplified rule of thumb is that the stronger you can make the muscles surrounding any given joint, the better they hold the joint together, and the more stability it will have.
Biomechanical studies of the spine have taught us that mechanical loads are transferred from the hips, pelvis, and low back, across the Thoracolumbar Fascia, to the upper back, shoulders, and arms, in an “X” shaped fashion (the thoracolumbar fascia is at the center of the X).
For instance, motions that involve twisting or rotating the trunk would transfer force up the right hamstring / gluteal muscles to the opposite side latissimus dorsi / trapezius (or visea versa). If you picture this occurring, the Thoracolumbar Fascia would be at the center of the X. For more information, please read our posts on UPPER CROSSED SYNDROME and most particularly, LOWER CROSSED SYNDROME. For those of you struggling with chronic low back pain, you will not be able to begin helping yourself without understanding these simple concepts (not to mention, there is tons of self-help there).
MORE ON THE THORACOLUMBAR FASCIA
Once you begin to understand the way that loads and forces are transferred through the lumbar spine (lower back), you can start to see why local pain found in a wide range of areas (low back, BUTTOCKS / PIRIFORMIS, SACROILLIAC JOINTS, HIP FLEXORS (A particularly big deal for athletes that both sit a lot and kick — think school-aged soccer players here), ABS / OBLIQUES, HAMSTRING, TRAP / LEVATOR, etc) may very well be due to problems in the Thoracolumbar Fascia.
Because the Thoracolumbar Fascia is the center of the X, and virtually all trunk motion must be transferred through it, an injury to this particular tissue can prove catastrophic on many levels. Like many other injuries, the chief components of Thoracolumbar injury are inflammation, pain, loss of strength, loss of joint motion, and subsequent degeneration (HERE). Let’s tackle them one at a time. But before we do that, I want to talk just a moment about Fascia in general.
Fascia is the tough, yellowish-clear membrane that is found underneath the skin, and tightly covers any number of tissues, including muscles. A fun-fact that most practitioners are unaware of is that Fascia has the ability to contract (SLIGHTLY) similarly to muscle. Oh; and it actually acts as a second nervous system (HERE). Fascia can be responsible for all sorts of PAIN SYNDROMES, even though it cannot normally be seen with an MRI (HERE). In fact, if you want to see how cool this tissue really is, make sure to read my post, TWENTY FIVE REASONS WHY FASCIA or better yet, an organized conglomeration of all 165 of my fascia posts (HERE).
A 2009 study from the medical journal Spine shed some additional light on this topic of imaging Fascia. After trying to determine if problems of the Thoracolumbar Fascia could be seen using MRI, researchers at Philadelphia’s Rothman Institute at Thomas Jefferson University Hospital concluded that, “The sensitivity and specificity of MRI for diagnosing injury of the PLC [Thoracolumbar Fasica] are lower than previously reported in the literature. The integrity of the PLC [Thoracolumbar Fascia] as determined by MRI should not be used in isolation to determine treatment.” In other words, you might see it, but the image is not good enough to be considered ‘diagnostic’.
Stop and think about the gravity of this situation for a moment. The single most pain-sensitive tissue in your body is poorly imaged with current MRI technology (HERE). Furthermore, Scar Tissue in this area is a recipe for disaster because it can become hyper-sensitized to the point that some researchers say it is over 1,000 times more painful than normal tissue (HERE). This is the most logical reason as to why the latest research on back pain says that 85% of all low back pain is “NON-SPECIFIC” (it cannot be related back to a specific tissue or cause) — up from 75% just a few short years ago.
To better understand what I am talking about when I talk about SCAR TISSUE or FIBROSIS, you need to take a couple of minutes and look at the links. Now that you have an improved understanding of Fascia in general, we can cover the three chief components of injuries to the Thoracolumbar Fascia.
- PAIN: As many of you have discovered, low back pain, SCIATICA, buttock pain (PIRIFORMIS SYNDROME), and SACROILIAC JOINT PAIN do not always respond to repeated Chiropractic Adjustments. Don’t get me wrong; Chiropractic Adjustments are going to rapidly help many if not most people struggling with pain in these areas. But if there is one thing that I have learned over the past two decades of practice, it is that if Scar Tissue is present, you had better deal with it first if you want any sort of chance at achieving long-lasting pain relief. It is also important to understand that the Thoracolumbar Fascia is continuous with the CERVICAL (NECK) FASICA, which is continuous with SKULL FASCIA as well. In other words, it’s all attached to each other into a continuous sheath (HERE and HERE are insane examples). This means that problems in one area of the body have the potential to cause pain in distant areas of the body — one of several reasons that the most well known whiplash researchers on the planet stated almost two decades ago that the injuries seen in whiplash accidents are likely to cause, “bizarre and seemingly unrelated symptoms“. HEADACHES are just one of many common results of injury to the Thoracolumbar Fascia (you’ll see why momentarily).
- LOSS OF FUNCTION: As you will see in a moment, loss of motion / function (Functio Leasa — the fifth component of INFLAMMATION) is a huge component of a Fascial Injury and the subsequent Scar Tissue and Fibrosis that forms as a result. It also goes hand in hand with loss of strength. Both of these lead to that vicious cycle of pain and re-injury, which in turn, leads us to our next bullet point. In the video clips below, I want you to take note of the results of a study that was published just over a year ago. NIH’s National Center for Complementary and Alternative Medicine funded this study that was published in BMC Musculoskeletal Disorders back in 2011. The 10 second video clips are diagnostic Ultrasounds of Thoracolumbar Fascia — healthy (no low back pain) -vs- injured (low back pain). For those of you struggling with Chronic Pain, the difference is shocking. It is refreshing to see that the model I have been describing to patients for over two decades is right on target. The Fascial Adhesions as seen in THESE TWO TEN SECOND VIDEOS helps explain the mystery.
- DEGENERATION: The end product of loss of normal joint function (strength and motion) is degeneration. Yes, it’s true — if we live long enough, this becomes part of the normal aging process. However, because bony degeneration is so easily imaged with X-rays, MRI’s, or CT, it is a convenient scapegoat for pain — whatever kind of pain you may be having (HERE). In other words, it is easy to blame pain on Spinal Degeneration when the reality is that according to study after study, it probably has little or nothing to do with your pain (the chief reason I stopped taking x-rays a decade ago). To really understand Spinal Degeneration, you need to have a cursory understanding of the neurological component of this whole process —- MECHANORECEPTION / PROPRIOCEPTION. One more important fact to remember while we are on this topic; not only do the bones, discs, and cartilages in the area of a restricted Thoracolumbar Fascia degenerate, the Fascia itself degenerates. This is easy to understand when you realize that the Thoracolumbar Fascia is really an APONEUROSIS that is made up of several muscle tendons. In other words, the degeneration of the Thoracolumbar Fascia might almost be better understood in terms of TENDINOSIS rather than Fascial Adhesion
TOP TEN WAYS TO EFFECTIVELY DEAL WITH CHRONIC LOW BACK PAIN
The truth is, almost anyone, no matter what you have been through, or what you are currently going through, can help improve the health and biomechanical integrity of their spine. It is not only a matter of know-how, it is a matter of want-to and stick-to-it-iveness.
Yes, it can be tough — at least at first — to do what it takes to heal your back. This is because to truly heal your back, you have to address your entire body. It’s not just a matter of doing the ‘magic’ exercises, stretches, and therapy, while continuing to live a self-destructive lifestyle. All of this becomes particularly critical once you realize how poor a job standard diagnostic imaging (X-ray, CT, MRI) does as far as telling you what’s really wrong with your back (HERE and HERE).
- LOSE THE WEIGHT: If you are struggling with low back pain, but are not willing to do what it takes to get rid of excess weight (especially BELLY FAT, which puts massive mechanical torque on the low back), you are sabotaging your own efforts. I cannot tell you you how many patients tell me that if they gain just 10 extra pounds their back hurts. The best ways to lose weight are actually found on my clinic’s “Checklist Handout” HERE. By the way, I already know what you are thinking. You want me to know that you cannot lose the weight because the pain keeps you from exercising. This EXCUSE does not fly here. Weight loss is 80-90% diet, which means it is only 10-20% exercise. If you follow my advice, you can accomplish weight loss without exercise. Be aware though, that losing weight may mean an increased emphasis on Gut Health.
- HEAL YOUR GUT: Because virtually all health problems have a UNIVERSAL CAUSE, it would be in your best interest to learn about it and understand it. GUT HEALTH is critical for overall health, whether we are talking about your back, your THYROID, or your, ADRENAL GLANDS, or anything else. For decades, natural healers have said, “heal the gut, heal the body.” An understanding of Gut Health begins with a thorough understanding of LEAKY GUT SYNDROME and DYSBOSIS.
- CONTROL INFLAMMATION: The first thing you have to understand in your quest to heal your back is that INFLAMMATION, while probably a huge part of your problem, is probably not what you think it is (swelling). HERE is great information on eating an Anti-inflammatory Diet. And if you are still smoking; stop it already! Smoking is not only highly Inflammatory, it literally starves every cell in your body for OXYGEN. For those who think that this bullet is not critical, the March 2015 issue of the European Journal of Pain (Inflammation of the Thoracolumbar Fascia Excites and Sensitizes Rat Dorsal Horn Neurons) concluded that, after rats had their TL Fascia exposed to inflammation, “the expansion of the spinal target region of fascia afferents [sensory nerves]… and the appearance of new receptive fields is a possible explanation for the spread of pain in patients with non-specific low back pain.” In other words, inflammation created more nerves to sense pain. Bottom line, if you are not controlling inflammation without drugs, this will always lead to degenerative changes of the spine and surrounding tissues (HERE).
- CONTROL YOUR BLOOD SUGAR: How many health problems are being tied back to UNCONTROLLED BLOOD SUGAR? Thanks to inflammation, just about all of them. If you fail to understand this point (even if your blood sugar is ‘normal’), your ability to heal your spine will be severely hampered — even without DIABETES. Much of this is due to the extreme damage caused by the by-product of sugar metabolism — AGES (Advanced Glycation Endproducts). By the way, the diet I recommend for this and each of the preceding bullet points? PALEO — particularly critical for those who are dealing with a SYSTEMIC FASCIA PROBLEM. Be aware that KETOGENIC can prove effective as well.
- MAKE SURE THERE IS NO SCAR TISSUE PRESENT: No need for expensive diagnostic testing as far as this is concerned. It is crucial to understand that the things mentioned in the previous bullet point will not work if the Thoracolumbar Fascia contains SCAR TISSUE (aka “FIBROSIS“). If you are having Chronic Low Back Pain, make sure you try a couple of TISSUE REMODELING TREATMENTS! Re-watch the earlier-mentioned videos if you need to understand this concept better.
- WATCH YOUR POSTURE: Posture used to be a big deal. It used to be taught in school. Now it is all but ignored. POSTURE is not difficult, but you’ll have to strengthen your core (more to come on this shortly).
- DO NOT SIT TOO MUCH: When you sit down, you take the load off your feet and put it on your spine — most particularly your low back. In fact, sitting puts four times the amount of mechanical pressure / stress on your back as does standing. If you have a desk job, you may want to consider a stand up desk of some sort. Getting your screen up high helps keep you from slumping, as does sitting on an exercise ball instead of a chair (see bullet on core strength below).
- MAKE SURE TO MOVE EARLY AND OFTEN: Walk, swim, bike, get on an elliptical, use a TRAMPOLINE, buy a WHOLE BODY VIBRATION MACHINE. I don’t really care what you do, just move. We discussed earlier how loss of joint motion creates all sorts of problems in the low back. And finally, do not neglect adding a STRENGTH PROTOCOL to your program. After the age of 30 people lose 10% of their muscle mass per decade for the rest of their lives — unless they are actively and aggressively working their muscles against resistance.
- STRENGTHEN YOUR SPINE AS WELL AS YOUR ENTIRE BODY: I would suggest a regimen of CORE STRENGTHENING TECHNIQUES to start with. Talk to me before proceeding from there. See our previous links on Upper Crossed Syndrome and Lower Crossed Syndrome as well for any number of yoga-like stretches and core exercises.
- GET AN INVERSION TABLE: This helps a lot of people struggling with low back pain. HERE is my blog post on the topic.
- TRY SPINAL DECOMPRESSION THERAPY: There is great evidence that SPINAL DECOMPRESSION THERAPY can help 60-70% of you who are struggling with severe back issues such as Disc Problems, Spinal Stenosis, Facet Syndrome, or Spinal Degeneration. Be aware that it will most likely require Scar Tissue Mobilization to effectively deal with the Thoracolumbar Fascia.
- OTHER: I have another article on the same subject that approaches this from a bit different direction (HERE). Oh, and for those of you who are interested, I’ve included my solve-it-all super post (HERE), just for good measure! And if you appreciate what I am doing here, be sure and like, share of follow on FACEBOOK!
